This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Glowing dye may help surgeons eradicate prostate cancer

A glowing marker dye that sticks to prostate cancer cells could help surgeons to remove them in real-time, according to a paper published in the European Journal of Nuclear Medicine and Molecular Imaging, titled "First‑in‑man study of the PSMA Minibody IR800‑IAB2M for molecularly targeted intraoperative fluorescence guidance during radical prostatectomy."
Scientists, based at the Nuffield Department of Surgical Sciences and the Department of Oncology, University of Oxford, Oxford University Hospitals and Oxford NIHR Biomedical Research Center used a fluorescent dye attached to a special marker molecule to give medics a "second pair of eyes" during surgery for prostate cancer.
Twenty-three men with prostate cancer were injected with the marker dye before undergoing prostate removal surgery. The marker dye found areas of cancerous tissue not picked up by the naked eye or other clinical methods.
The dye allowed the surgeons to remove all cancerous tissues—which could reduce the chances of cancer coming back—while preserving healthy tissues. Preserving healthy tissues means fewer life-changing side effects after surgery.
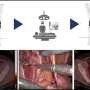
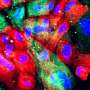
The combination of dye and targeting molecule, called IR800-IAB2M, allows surgeons to see the edges of the tumor and identify any clusters of cells that have spread from the tumor into nearby pelvic tissues and lymph nodes. This guides the surgeon to remove all cancerous tissues and preserve healthy areas around the prostate.
This substantially reduces the chances that the cancer will come back in future and minimizes the possibility of life changing side-effects for the patient after the operation.
The dye and marker molecule work by attaching themselves to a protein called Prostate-Specific Membrane Antigen (PSMA) commonly found on the surface of prostate cancer cells.
The marker molecule is made from a smaller version of an antibody called a "minibody," which can only bind to PSMA and not to any other molecule. The dye and marker molecule combination were developed by Oxford scientists in collaboration with ImaginAb Inc., a company based in Inglewood, California.
In the first stage of the ProMOTE study, 23 men diagnosed with prostate cancer were injected with the fluorescent dye before undergoing robot-assisted surgery to remove the prostate (known as a radical prostatectomy).
Surgeons used an imaging system that shines a special type of light on the prostate and nearby areas, to make the prostate cancer cells glow. The imaging system was developed by an engineering team led by Professor Borivoj Vojnovic at the University of Oxford.
For multiple patients in the study, the dye identified clusters of cells which had spread away from the tumor which couldn't be seen by the naked eye.
This marker dye is in its early stages of clinical development, but in future it could be used routinely by surgeons to see every part of the cancer while they perform surgery to remove the prostate.
The imaging system to see glowing cancer cells could be integrated into the robot-assisted tools used for prostate surgery. The marker dye could also be used for other types of cancer, by changing the protein it uses to attach itself to the cancer cells.
Further clinical trials are already underway in larger groups of patients to find out if the technique removes more prostate cancer, and preserves more healthy pelvic tissue, compared to existing surgical methods.
Prostate cancer is the most common cancer in men in the UK, with around 52,300 new cases every year.
Nuffield Professor of Surgery at the University of Oxford and lead author of the study, Professor Freddie Hamdy, said, "We are giving the surgeon a second pair of eyes to see where the cancer cells are and if they have spread. It's the first time we've managed to see such fine details of prostate cancer in real-time during surgery.
"With this technique, we can strip all the cancer away, including the cells that have spread from the tumor which could give it the chance to come back later. It also allows us to preserve as much of the healthy structures around the prostate as we can, to reduce unnecessary life-changing side-effects like incontinence and erectile dysfunction.
"Prostate surgery is life changing. We want patients to leave the operating theater knowing that we have done everything possible to eradicate their cancer and give them the best quality of life afterwards. I believe this technique makes that possibility a reality."
Executive Director of Research and Innovation at Cancer Research UK, Dr. Iain Foulkes, said, "Surgery can effectively cure cancers when they are removed at an early stage. But, in those early stages, it's near impossible to tell by eye which cancers have spread locally and which have not.
"We need better tools to spot cancers which have started to spread further. The combined marker dye and imaging system that this research has developed could fundamentally transform how we treat prostate cancer in the future.
"We hope that this new technique continues to show promise in future trials. It is exciting that we could soon have access to surgical tools which could reliably eradicate prostate and other cancers and give people longer, healthier lives free from the disease."
More information: European Journal of Nuclear Medicine and Molecular Imaging (2024). DOI: 10.1007/s00259-024-06713-x