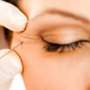
Could depression be treated with Botox?
In the largest randomized, double-blind, placebo controlled study to date on the effect of OnabotulinumtoxinA (as known as Botox) on depression, researchers found that more than half of subjects suffering from moderate to severe depression showed a substantial improvement (greater than or equal to 50% of baseline) in their depressive symptoms as measured by the MADRS scale.
The study, conducted by Dr. Eric Finzi, MD, PhD and Dr. Norman E. Rosenthal, MD and published in the Journal of Psychiatric Research, included 74 depressed subjects injected with a single treatment of either onabotulinumtoxinA (OBA) or a placebo to the corrugator and procerus muscles between the eyebrows. Results showed that depressive symptoms (as assessed by the MADRS scale) in the OBA treatment group decreased 47 percent after six weeks, compared to 21 percent in the placebo group. This study is the first to show a significant difference in remission rate with OBA in depressed patients (27% OBA vs. 7% placebo).
Study co-author Dr. Norman E. Rosenthal, MD, Clinical Professor of Psychiatry at Georgetown Medical School, commented, "This research is groundbreaking because it offers those who suffer from depression and their doctors an entirely new approach to treating the condition - one that doesn't conflict with any other treatments."
The study showed that Botox may help relieve depressive symptoms both as a stand-alone and an adjunctive treatment.
"This new research supports earlier facial feedback theory of Charles Darwin and William James which suggests that facial expressions influence mood," added Dr. Eric Finzi, Dermasurgeon and co-author on the paper that first reported that inhibition of frowning by facial injection of OBA could help depressed patients in a pilot study published in 2006.
More information: This article "Treatment of depression with onabotulinumtoxinA: A randomized, double-blind, placebo controlled trial" by Eric Finzi and Norman E. Rosenthal, is published in Journal of Psychiatric Research, Volume 52 (May 2014). dx.doi.org/10.1016/j.jpsychires.2013.11.006