Researchers pilot educational and behavioral program to reduce lymphedema risk
Viewed as one of the most unfortunate outcomes of breast cancer treatment, lymphedema is characterized by an accumulation of lymph fluid in the interstitial spaces of the affected limb, leading to chronic ipsilateral limb swelling causing psychosocial distress and physical challenges for patients.
Even conservative estimates suggest that 3% of women who have had sentinel lymph node biopsy and 20% of those who have had axillary lymph node dissection may develop lymphedema a year after breast cancer surgery. Two established risk factors for lymphedema are compromised lymphatic drainage and higher body mass index (BMI).
To date, there is little high-quality evidence to support the role of precautionary life-style strategies in reducing these risk factors.
Now, a team of researchers led by Mei R. Fu, PhD, RN, ACNS-BC, FAAN, associate professor of Chronic Disease Management at the New York University College of Nursing (NYUCN) conducted a pilot study to evaluate a patient-centered educational and behavioral self-care program called The Optimal Lymph Flow. The goals of the program were to promote lymph flow and optimize BMI over a 12-month period after breast cancer surgery. Findings of the study entitled "Proactive Approach to Lymphedema Risk Reduction: A Prospective Study" was published first on-line in the Annals of Surgical Oncology (May 2014). They offer initial evidence in support of a shift in the focus of lymphedema care away from treatment and toward proactive risk reduction.
"A patient-centered educational and behavioral program focusing on self-care strategies appears to be an effective way to reduce the risk of lymphedema in survivors of breast cancer," said Dr. Fu. "Based on these study findings, the New York University College of Nursing has established this patient-centered lymphedema risk reduction program as a web-based avatar technology intervention."
Dr. Fu's team enrolled 140 women and followed them for 12 months after surgery for breast cancer. Women who had metastatic breast cancer, a history of breast cancer and lymphedema, or bilateral breast cancer were excluded from the study.
Nearly 60% of patients had undergone axillary lymph node dissection, and approximately 40% had undergone sentinel lymph node biopsy. Although more women in the dissection group had had a mastectomy and chemotherapy than in the biopsy group, both groups were similar in terms of body weight and BMI.
The educational and behavioral program consisted of an assortment of self-care strategies. They included shoulder mobility exercises, muscle-tightening deep breathing, muscle-tightening pumping exercises, and large-muscle exercises to promote lymph flow and drainage (eg, walking, marching, dancing, swimming, yoga, tai chi). In addition, to maintain their preoperative BMI, the women were offered nutritional instructions and encouraged to follow a balanced, portion-appropriate diet.
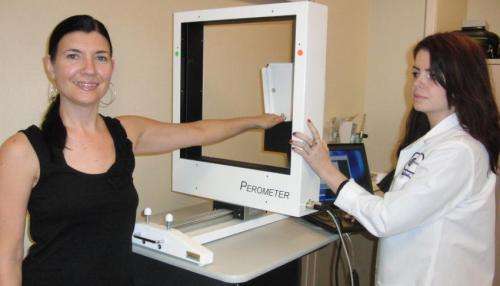
Limb volume change assessed by an infrared perometer and BMI via a bioimpedance device were outcome measures. Assessments were performed before surgery (baseline) and after surgery (at 2-4 weeks, 6 months, and 12 months). Lymphedema was defined as ≥ 10% increase in limb volume from baseline in the ipsilateral arm compared with changes in the contralateral arm.
Of the 134 women who completed the study, 97% of patients maintained and improved their preoperative limb volume and BMI at 12 months after surgery. No patients exceeded a 10% increase in limb volume at 12-month follow-up. No patients reported injury or discomfort associated with The Optimal Lymph Flow program at any follow-up visit, according to the investigators.
"The Optimal Lymph Flow Program promotes lymph flow and optimal [BMI] by empowering, rather than inhibiting, how survivors live their lives," said Dr. Fu. "Its underlying premise is 'what to do' rather than 'what to avoid."
These preliminary findings suggest that self-care strategies such as The Optimal Lymph Flow program may prove to be an effective way to reduce the risk of lymphedema in survivors of breast cancer. In fact, nearly 90% of the women studied reported that the program helped them to understand how to reduce their risk of lymphedema as well as dispel their fear and anxiety about developing this side effect. Future research requires a larger study with a randomized, controlled design to confirm the program's overall benefits.
More information: Paper: http://www.annsurgoncol.org/journals/abstract.html?v=0&j=10434&i=0&a=3761_10.1245_s10434-014-3761-z&doi=