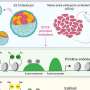
Healthcare professionals must be aware of rarer causes of headaches in pregnancy
Most headaches in pregnancy and the postnatal period are benign, but healthcare professionals must be alert to the rarer and more severe causes of headaches, suggests a new review published today in The Obstetrician & Gynaecologist (TOG).
The review looks at common causes for headaches during pregnancy and the postnatal period, possible conditions that may be associated with headaches and how healthcare professionals should manage the care of the woman appropriately.
There are 85 different types of headache. Approximately 90% of headaches in pregnancy are migraine or tension-type headaches. However, pregnancy can lead to an increased risk of certain secondary headaches, a headache caused by an underlying health condition, states the review.
The review states that most headaches in pregnancy are benign but in some cases can be more serious. According to the Confidential Enquiries into Maternal Deaths in the United Kingdom 2006 – 2008 report, neurological conditions were the third most common cause of death, considering both direct and indirect causes. The authors of the review therefore emphasise the need for all medical staff to be well trained to take a full history and examination, make a provisional differential diagnosis and know when to seek neurological expertise.
Migraine is a common form of headache; the condition is more common in women, with the highest prevalence rates during the childbearing years. The review states that pregnancy leads to a reduction in the frequency and severity of attacks of migraines without aura, also known as a common migraine. However, women who do experience migraines have a more than two-fold increased risk of pre-eclampsia than those who do not. Women therefore need to be aware to consult a healthcare professional if their headache is different from their usual migraine, highlights the review.
Another condition associated with a headache in pregnancy is idiopathic intracranial hypertension, a build up of high pressure inside the skull, a rare condition but more prevalent in obese women of childbearing age. The condition may present for the first time in pregnancy and pre-existing disease tends to worsen in pregnancy. It can be fatal if it is not treated promptly as a medical emergency.
Pregnancy is also a recognised risk factor for cerebral venous thrombosis (CVT), the presence of a blood clot in the dural venous sinuses, which drain blood from the brain. Caesarean section, systematic infection, vomiting and anaemia increase the risk and headache is the most frequently (80 – 90%) occurring symptom in CVT and often the first symptom reported by patients.
The review also discusses imaging and advises that imaging of the brain should never be withheld because a woman is pregnant and women should be reassured that imaging is safe.
Kirsty Revell, Specialist Registrar, Obstetrics and Gynaecology at the Princess Anne Hospital, Southampton and co-author of the review said:
"Headaches are common in life and in pregnancy. Most headaches are benign, for example migraine or tension headaches, but some headache types can be more serious and an indication that something is seriously wrong.
"It is vital that both GPs and obstetricians are aware of the signs and symptoms associated with these conditions and know when to seek advice from a specialist."
Jason Waugh, TOG Editor-in-chief added: "Many women experience headaches during pregnancy and the postpartum period and most are managed by women themselves or within primary care.
"Women presenting with headaches in pregnancy and the postnatal period may be at home, on a maternity ward, in an antenatal clinic, at a tertiary referral centre or in an emergency department. All medical staff should be aware of the symptoms, signs and appropriate response to the rarer and more severe causes of headaches that continue to cause avoidable morbidity and mortality."
More information: K Revell, P Morrish. Headaches in pregnancy. The Obstetrician & Gynaecologist 2014; dx.doi.org/10.1111/tog.12101