Vitiligo treatment holds promise for restoring skin pigmentation
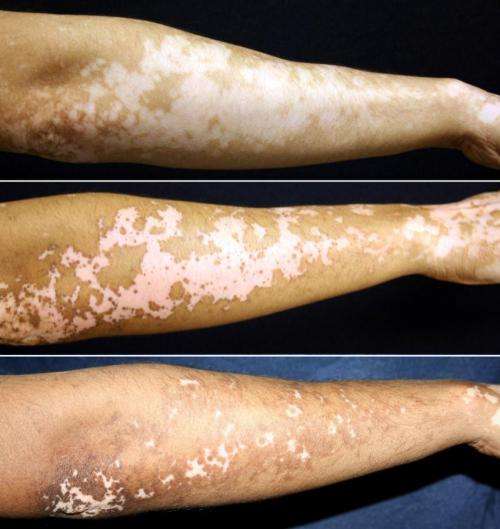
A treatment regimen is safe and effective for restoring skin pigmentation in vitiligo patients, according to a Henry Ford Hospital study.
"Our findings offer patients with vitiligo worldwide a renewed hope for a bright future in the treatment of this disfiguring disease," says Henry Lim, M.D., chair of Dermatology at Henry Ford and the study's lead author. "Patients with lesions on their face and arms could have a more rapid response to the combination treatment."
Henry Ford dermatologists described the repigmentation results as "superior," and said the treatment combination holds promise as a future therapy for the more than 50 million people worldwide living with vitiligo. It affects about one in every 100 people in the United States.
The study will be published online Wednesday in the Journal of the American Medical Association-Dermatology.
In a multi-center study led by Henry Ford, dermatologists sought to evaluate the safety and effectiveness of a treatment combination of afamelanotide, a drug that induces skin pigmentation, and phototherapy using narrowband ultraviolet-B rays (NB UVB). Phototherapy, or ultraviolet light therapy, is the treatment of choice for many patients with widespread vitiligo. It has been shown to be effective, though the degree of repigmentation varies.
Dr. Lim, an international vitiligo expert, says afamelanotide "enhances the ability of the UVB to induce repigmentation of the skin."
Patients were randomly divided into two study groups: Group A received the combination therapy; Group B received only NB UVB treatment.
Key findings:
- Repigmentation occurred faster in patients who received the combination treatment compared to patients who received NB UVB.
- Patients who received the combination treatment achieved appearance of pigment on their face and arms after 40 days compared to 60 days for patients who received NB UVB.
- In dark-skinned patients, repigmentation occurred faster in the combination group compared to the NB UVB group.
Afamelanotide is in the process of being submitted for approval from the U.S. Food and Drug Administration for use in treating vitiligo.
Vitiligo is a skin disease that causes the skin to lose color and develop white patches that vary in size and location. It develops when cells called melanocytes are killed by the body's immune system, causing the area of skin to turn white because the cells no longer make pigment. Vitiligo is more noticeable in individuals with darker skin tones, but it affects all races and ethnicities.
While vitiligo is neither contagious nor life-threatening, there is no cure. However, it causes low self-esteem and depression for those living with the disease.
The Henry Ford study represents its latest research into investigating new treatment options for vitiligo. In a 2012 study published in the Journal of the American Academy of Dermatology, Henry Ford dermatologists showed the benefits of skin cell transplant surgery, called melanocyte-keratinocyte transplantation or MKTP. Henry Ford has since performed more than 190 MKTP procedures on patients from Michigan, 23 other U.S. states and Canada.
For this new study, 55 patients were enrolled at four sites – Henry Ford, Icahn School of Medicine at Mount Sinai in New York and Vitiligo and Pigmentation Institute of Southern California and University of California Davis' Department of Dermatology.
In the two study groups, 28 patients were enrolled in Group A and 27 patients in Group B. Both groups received phototherapy two to three times a week for six months for a total of 72 treatments. In addition to phototherapy, patients in Group A received a dose of 16 mg of afamelanotide in four monthly treatments. Afamelanotide, about the size of a grain of rice, was implanted just under the skin.
Two common vitiligo assessment scoring systems – Vitiligo Area Scoring Index and Vitiligo European Task Force – were used to evaluate the repigmentation response.
While patients in both groups showed repigmentation, the response in Group A was superior to Group B by the 56th day of treatment and even better by the 168th day of treatment. The most common side effect was redness of the skin.
More information: JAMA Dermatology. Published online September 17, 2014. DOI: 10.1001/jamadermatol.2014.1875


















