Mapping blood flow with bubbles and ultrasound
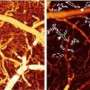
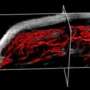
Microbubbles are being used with ultrasound to create microscopic maps of blood vessels, in a new technique being developed by King's College London and Imperial College London. This new approach, which generates much more detailed images than conventional ultrasound, may one day help doctors to spot early signs of blood vessel growth or damage, or establish whether a patient is responding to treatment.
Changes in blood circulation can be early indicators of the onset of conditions like diabetes and heart disease. In addition, the formation of new blood vessels can play a vital role in the growth and spread of tumors and is therefore an important predictor of how some cancers will develop.
Ultrasound is a non-invasive way of studying the body internally, but the resolution is fundamentally limited by the wavelength of the sound used to form the image. There is also a trade-off between how deep you can image into the body and how detailed the images will be. The method, published in the journal Transactions on Medical Imaging, was used to visualize micro-vascular blood flow in mice for the first time and reveals fine structure not previously seen with conventional ultrasound.
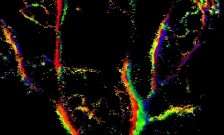
In the study, the team combined standard ultrasound imaging with the use of microbubbles and computer processing to 'map' blood vessels in the ear of a mouse. By ensuring that only a small number of bubbles were present in the image at any one time, they were able to determine the position of each microbubble far more accurately than is normally possible. By also tracking the tiny bubbles injected into the bloodstream – measuring how fast and in what direction each bubble was moving – the team was able to generate a map showing the speed and direction of blood flow through the vessels. The 'super-resolved' images provided much more detailed information compared with those produced by conventional ultrasound.
The next stage of this research will be to extend the method's capability to full 3D imaging and speed up the technique enabling images to be captured and interpreted in real time – in this study, it took around 10 minutes to generate the super-resolved images.
The microbubbles used in the study were similar in size to red blood cells – less than ten microns in diameter – and acted as 'markers' for the presence of blood vessels.
Dr Robert Eckersley, lead author in the Division of Imaging Sciences & Biomedical Engineering at King's College London, says: "Microbubbles are already used in hospitals to produce clearer images in body scans, but have the potential to help us gather much more useful information from a patient. If we can develop better ways of producing super-resolved images in the clinic, this would help doctors to detect diseases like cancer at an earlier stage, and follow in greater detail how a patient is responding to therapy."
More information: "In Vivo Acoustic Super-Resolution and Super-Resolved Velocity Mapping Using Microbubbles," IEEE Transactions on Medical Imaging, ieeexplore.ieee.org/xpl/abstra … rue&arnumber=6908009