Patient's own stem cells could clear a cloudy cornea, study says

Treating the potentially blinding haze of a scar on the cornea might be as straightforward as growing stem cells from a tiny biopsy of the patient's undamaged eye and then placing them on the injury site, according to mouse model experiments conducted by researchers at the University of Pittsburgh School of Medicine. The findings, published today in Science Translational Medicine, could one day rescue vision for millions of people worldwide and decrease the need for corneal transplants.
According to the National Eye Institute, part of the National Institutes of Heath, "Worldwide, corneal infectious diseases have compromised the vision of more than 250 million people and have blinded over 6 million of them." Trauma, such as burns, are also a leading cause of corneal scarring, said senior investigator James L. Funderburgh, Ph.D., professor of ophthalmology at Pitt and associate director of the Louis J. Fox Center for Vision Restoration of UPMC and the University of Pittsburgh, a joint program of UPMC Eye Center and the McGowan Institute for Regenerative Medicine.
"The cornea is a living window to the world, and damage to it lead to cloudiness or haziness that makes it hard or impossible to see," Dr. Funderburgh said. "The body usually responds to corneal injuries by making scar tissue. We found that delivery of stem cells initiates regeneration of healthy corneal tissue rather than scar leaving a clear, smooth surface."
Study lead author Sayan Basu, MBBS, MS, a corneal surgeon working at the L.V. Prasad Eye Institute in Hyderabad, India, joined Dr. Funderburgh's lab in Pittsburgh. Dr. Basu had previously developed a technique to obtain ocular stem cells from tiny biopsies at the surface of the eye and a region between the cornea and sclera known as the limbus. Removal of tissue from this region heals rapidly with little discomfort and no disruption of vision. After collecting biopsies from banked human donor eyes, the team expanded the numbers of cells in a culture plate using human serum to nourish them. They conducted several tests to verify that they these cells were, in fact, corneal stem cells.
"Using the patient's own cells from the uninjured eye for this process could let us bypass rejection concerns," Dr. Basu noted. "That could be very helpful, particularly in places that don't have corneal tissue banks for transplant."
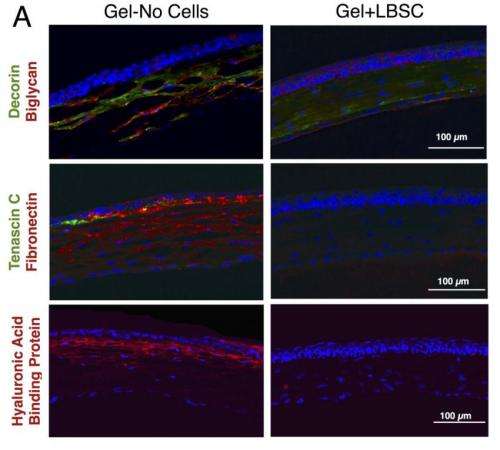
The team then tested the human stem cells in a mouse model of corneal injury. They used a gel of fibrin, a protein found in blood clots that is commonly used as a surgical adhesive, to glue the cells to the injury site. They found the scarred corneas of mice healed and became clear again within four weeks of treatment, while those of untreated mice remained clouded.
"Even at the microscopic level, we couldn't tell the difference between the tissues that were treated with stem cells and undamaged cornea," Dr. Funderburgh said.
"We were also excited to see that the stem cells appeared to induce healing beyond the immediate vicinity of where they were placed. That suggests the cells are producing factors that promote regeneration, not just replacing lost tissue."
His team's work is the inspiration behind a small pilot study underway in Hyderabad in which a handful of patients will receive their own corneal stem cells as a treatment.
More information: "Human limbal biopsy–derived stromal stem cells prevent corneal scarring in mice," by S. Basu et al. Science Translational Medicine, stm.sciencemag.org/lookup/doi/ … scitranslmed.3009644