Early intervention program for psychosis demonstrates effectiveness
Providing comprehensive coordinated care to young people after they experience a first episode of psychosis can help them avoid hospitalization and resume their school and work lives, according to research published today in Psychiatric Services in Advance, a publication of the American Psychiatric Association.
Many clinicians and researchers now regard the first years after psychosis onset as "a window of opportunity" during which evidence-based interventions can stop the downward spiral of functional loss long thought to be the only outcome for people with schizophrenia. In this first U.S. controlled trial of an early intervention model, researchers compared 120 patients randomly assigned to treatment at the clinic for Specialized Treatment Early in Psychosis (STEP) to usual treatment. The STEP clinic, located at the Connecticut Mental Health Center, is a partnership between Yale University and the Connecticut Department of Mental Health and Addiction Services.
STEP provides comprehensive care to patients and their families after a first episode of psychosis, which often occurs in late adolescence or early adulthood. STEP participants in the study chose from an array of services, including psychotropic medications, family education, cognitive-behavioral therapy (CBT), and case management with employment and educational support. The care of each STEP patient was carried out by a team consisting of staff and trainees from psychiatry, psychology, social work and nursing. The team took a collaborative approach to coordinating care and targeted services to the needs of patients and families.
Patients assigned to usual treatment either continued treatment with existing outpatient providers or were referred on the basis of health insurance coverage. Patients eligible for public-sector care at the health center were referred per routine to one of the ambulatory teams at the center.
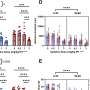
After one year in the STEP program, participants had fewer hospitalizations than those in the usual-care group. More than three-quarters of STEP participants avoided hospitalization, compared with about half of the usual-care group. And when STEP participants were hospitalized, their hospital stays were significantly shorter than those in the usual-care group.
In addition, STEP participants experienced greater improvements in vocational and educational functioning—79 percent of the STEP participants were employed or in school at one year, compared with 47 percent for the usual-care group. A third of patients in usual care dropped out of the labor force, compared with only 8 percent of STEP patients. In addition, STEP participants showed improvements in community functioning and were more likely to be in contact with outpatient mental health services.
"The model is a pragmatic, effective and economically feasible approach to early psychosis and one that is feasible to implement in real-world U.S. settings," said Vinod Srihari, associate professor of psychiatry at Yale and lead author of the study. "The message is simple: Treatment is available, effective, and the earlier, the better."
More information: "First-Episode Services for Psychotic Disorders in the U.S. Public Sector: A Pragmatic Randomized Controlled Trial" dx.doi.org/10.1176/appi.ps.201400236