April 7, 2015 report
Research effort leads to mammalian heart tissue regeneration
(MedicalXpress)—A large team of researchers with affiliations in Israel and Australia has found a way to cause cell regeneration in mice. In their paper published in the journal Nature Cell Biology, the team reports on their groundbreaking study of hormones, heart cell division and tissue regeneration.
One of the sad facts of life is that damage to the heart is permanent—if someone has the type of heart attack caused by blood vessel blockage, it generally means they sustain damage to heart tissue, and heart tissue, unlike other parts of the body is not regenerated. Instead, the person lives the rest of their lives with damage, unless they get a heart transplant.
Why heart muscle does not regenerate has been the subject of much research—some suggest it has something to do with our immune system—scientists have discovered that the cells in the heart go into a dormant state shortly after birth and that is why they do not divide, preventing repair of damaged tissue from occurring. In this new effort the researchers found a way to awaken the cells in the heart to allow them to divide and thus regenerate tissue. They discovered that if they stimulated a signaling system in the heart, which they already knew was driven by a hormone called neuregulin, it caused the heart cells to awaken and to begin dividing. They report that with mice that were caused to have heart damage due to blocked arteries, the approached worked almost flawlessly—the hearts were restored to nearly their prior condition.
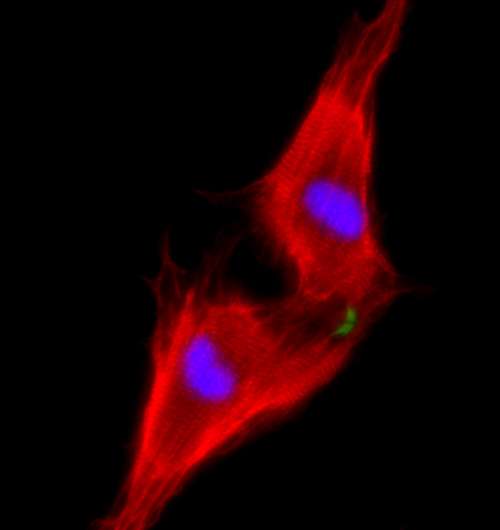
The results described by the researchers are big news, both for the medical community and for people in the future who experience heart damage, though there are some hurdles to overcome. Right now it is not known if the same approach would work with humans, and sadly, it is not feasible to stimulate signaling in live patients with neuregulin—doing so would almost certainly lead to other unpredictable results. Thus, the team has turned to looking for other ways to stimulate the same type of heart signaling to see if perhaps another drug, perhaps one that is already on the market, might do the trick. The team estimates that even if everything goes right, it would still be nearly a decade before a therapy would be available for patients.
More information: ERBB2 triggers mammalian heart regeneration by promoting cardiomyocyte dedifferentiation and proliferation, Nature Cell Biology, http://www.nature.com/articles/DOI:10.1038/ncb3149
Abstract
The murine neonatal heart can regenerate after injury through cardiomyocyte (CM) proliferation, although this capacity markedly diminishes after the first week of life. Neuregulin-1 (NRG1) administration has been proposed as a strategy to promote cardiac regeneration. Here, using loss- and gain-of-function genetic tools, we explore the role of the NRG1 co-receptor ERBB2 in cardiac regeneration. NRG1-induced CM proliferation diminished one week after birth owing to a reduction in ERBB2 expression. CM-specific Erbb2 knockout revealed that ERBB2 is required for CM proliferation at embryonic/neonatal stages. Induction of a constitutively active ERBB2 (caERBB2) in neonatal, juvenile and adult CMs resulted in cardiomegaly, characterized by extensive CM hypertrophy, dedifferentiation and proliferation, differentially mediated by ERK, AKT and GSK3β/β-catenin signalling pathways. Transient induction of caERBB2 following myocardial infarction triggered CM dedifferentiation and proliferation followed by redifferentiation and regeneration. Thus, ERBB2 is both necessary for CM proliferation and sufficient to reactivate postnatal CM proliferative and regenerative potentials.
© 2015 MedicalXpress.com