Proteomics provides new leads into nerve regeneration
Using proteomics techniques to study injured optic nerves, researchers at Boston Children's Hospital have identified previously unrecognized proteins and pathways involved in nerve regeneration. Adding back one of these proteins—the oncogene c-myc—they achieved unprecedented optic nerve regeneration in mice when combined with two other known strategies. The findings were published online April 30 by the journal Neuron.
Researchers have been trying for many decades to get injured nerves in the brain and spinal cord to regenerate. Various molecules have been targeted and found to yield nerve growth, but many studies have been hard to replicate. Even with most effective manipulations, the "holy grail" of regenerating a nerve enough for it to resume its function has been largely elusive.
"The majority of axons still cannot regenerate," says Zhigang He, PhD, co-senior investigator on the paper and a member of the F.M. Kirby Neurobiology Center at Boston Children's Hospital. "This suggests we need to find additional molecules, additional mechanisms. The proteomics approach fills the gap very well."
Studying mice with optic nerve injury—a classic, easy-to-study type of central nervous system injury—He and co-senior investigator Judith Steen, PhD, also of the Kirby Center, applied quantitative mass spectrometry to identify and quantify proteins produced by the injured retinal ganglion cells (RGCs), which run from the retina to the brain. Their team, including fellows, Stephane Belin, PhD, and Homaira Nawabi, PhD, used bioinformatics analyses to compare the protein measurements with those in intact RGCs and looked for patterns indicating proteins that act together in concert.
"This approach gave us a nice 30,000-foot view of what pathways are changed in the system as a whole in response to injury," says Steen. "It showed us the main pathways we should perturb to get regeneration."
The pathways matched many that were previously identified, but also included some new players, such as c-myc, TGF-b, NFkb, and Huntingtin, that could lead to a much better understanding of how to recover nerves' regenerative ability. "You may have to invoke several pathways simultaneously," says Steen. "You can't say there's one magic bullet."
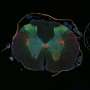
When the researchers induced mice to make more c-myc, optic nerve regeneration was promoted, even when some time had elapsed after the injury. When they combined this approach with deletion of two other molecules known to inhibit regeneration (PTEN and SOCS3), they saw a synergistic effect. The RGCs' survival was dramatically improved and their axons grew to the optic chiasm (the part of the brain where the optic nerves cross) and beyond—an unprecedented degree of regeneration. (See image)
The researchers caution that there is risk in stimulating c-myc (a tumor promoter) and deleting PTEN (a tumor suppressor), as both strategies could also promote cancer—the likely reason that these pathways are shut down once our nervous system has developed. However, there may be ways to mimic these pathways, or ways of stimulating them in a targeted, temporary fashion, the researchers suggest.
Steen and He note that microarray analyses, looking at what genes are transcribed (turned on) in injured nerves, have also been useful in identifying possible nerve regeneration strategies. The problem, Steen says, is that even when the genes are transcribed, the cell may not actually build the proteins they encode. "By measuring proteins, you get a more direct, downstream readout of the system," she says.
Steen and He are now testing other proteins they identified through their analysis and are finding some regenerative promise. They are also using proteomics to look for new pathways to target in other neurologic disorders such as Alzheimer's disease, frontotemporal dementia, spinal muscular atrophy and amyotrophic lateral sclerosis, as well as sensory nerve injury.