Researchers report success in mitigating treatment-related side effects in childhood leukemia

Ten-year-old Matty Hayes is among the 90 percent of kids who are still alive five years after being treated for leukemia. But he's also among the 60 percent who suffer severe side effects from the intense chemotherapy that saves their lives.
The problem with conventional chemotherapeutic drugs is that they don't differentiate between actively growing normal cells in children and uncontrollably dividing cancer cells, so they flood the entire body with highly toxic chemicals.
Hayes' mother, Cheryl, reports that her son experienced hair loss, plummeting energy levels, mood swings and muscle fatigue during his treatment. "I'm most concerned about late term effects that may affect his organs and especially his ability to learn," she says.
Now, a team of researchers from the University of Delaware, Nemours/A.I. duPont Hospital for Children and Jefferson Medical College has reported success with a targeted treatment approach that delivers anticancer medication directly to leukemic cells using nanoparticles.
The research is documented in a paper published in the current issue of Molecular Pharmaceutics, an American Chemical Society journal.
Although nanomedicine has advanced to clinical trials for adult cancer therapy, the field is still in its infancy for treatment of childhood malignancies such as acute lymphoblastic leukemia (ALL), which is what Hayes was diagnosed with at the age of two-and-a-half. ALL accounts for a third of deaths in children and adolescents affected by blood cancers.
"Nanotherapy offers multiple advantages over conventional therapy," says Vinu Krishnan, who was a doctoral student in UD's Department of Materials and Science Engineering when the research was done. "It facilitates targeted delivery and enables controlled release of drugs to reduce treatment-related side effects."
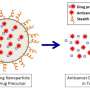
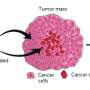
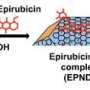
With this approach, tiny particles—ranging from 50 to 200 nanometers in size—are packed with drugs for targeted delivery to tumor cells, which engulf the particles, releasing the drug inside.
Since the drug is encapsulated and released slowly, nanoparticle-mediated drug delivery allows the use of low doses of the drug for treatment. However, one of the problems with this approach is that even normal cells engulf nanoparticles containing drugs.
To reduce the delivery of drugs into normal cells, the surface of drug-loaded nanoparticles can be adorned with sensor molecules that differentiate cancer cells from normal cells. Specific targeting of cancer can therefore mitigate side effects, since the drug is delivered primarily to the cancer cells.
"The success of survival rate in treating childhood cancers has greatly diminished funding for research in this area, and hence new therapeutic approaches are rarely implemented," says Ayyappan Rajasekaran, adjunct professor in materials science and engineering.
"Although the study is in the early stages, the data support the development of such approaches to treat pediatric cancers," he adds. "Enhanced funding to support the application of novel technologies to reduce treatment-related side effects in pediatric oncology is necessary to the well being of childhood cancer survivors."
Cheryl Hayes is grateful that Matty survived cancer and seems to have emerged from chemotherapy relatively unscathed.
"But it would be wonderful to have a treatment that reduced the side effects," she says. "It's difficult enough to face cancer in a young child—the side effects of the medication just add to the misery."
More information: "CD19-Targeted Nanodelivery of Doxorubicin Enhances Therapeutic Efficacy in B-Cell Acute Lymphoblastic Leukemia." Mol. Pharmaceutics, Article ASAP DOI: 10.1021/acs.molpharmaceut.5b00071