Human urine helps prevent bacteria from sticking to bladder cells
Human urine contains factors that prevent a common culprit in urinary tract infections (UTIs), uropathogenic Escherichia coli bacteria, from properly attaching to bladder cells, a necessary step for infection. The research, published this week in mBio, the online open-access journal of the American Society for Microbiology, reveals a weakness that could be exploited to develop more effective, non-antibiotic treatments for UTIs.
"There is a pressing, unmet need when it comes to developing new and better ways to treat UTIs," says Scott Hultgren, the Helen L. Stoever professor of molecular microbiology at Washington University School of Medicine in St. Louis who oversaw the study. Of the 10 million cases of UTI in the US each year, approximately 1 million are chronic recurrent cases. Those cases are of particular concern, says Hultgren, because they often involve bacteria that have become resistant to multiple antibiotics used to fight these infections.
"This study gives us a better understanding of the mechanism by which bacteria are able to colonize the urinary tract," says Hultgren. "Like an electrician, we have a molecular blueprint of the process and we can try to find a node to short-circuit the pathogenic cascade."
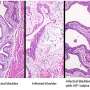
Hultgren's laboratory studies the uropathogenic E. coli (UPEC) bacteria that cause the vast majority of UTIs. A single UPEC bacterium can have hundreds of tiny hair-like structures called type 1 pili that help it attach to the walls of the bladder. The pili tips are made of FimH adhesin, a protein that tightly binds to a mannose sugar molecule decorating the outer surface of bladder cells. This attachment triggers bacterial invasion of these cells.
"Once the bacteria are able to invade that bladder epithelial cell, it becomes a safe haven where the bacteria rapidly replicate and gain a foothold for infection in the bladder," says Hultgren.
His group took a closer look at the assembly of these pili structures so key to infection. Because bacteria found in human urine are often missing these pili, Hultgren's team wondered if something in the urine itself caused the bacteria to halt assembly of these structures. Pilus assembly is controlled by an entire set of genes called the fim operon, which can be switched to ON or OFF phases by different signals.
When the researchers looked at UPEC grown in human urine from healthy individuals, they found that something in the urine switched all the fim operons to the OFF mode and kept them there. However, if UPEC bacteria were already attached via FimH to bladder cells grown in a lab dish, urine lost this effect.
Upon further inspection, the team also found that unknown factors in urine interfere with the bacterial FimH protein's ability to adhere to cells. In addition, when FimH function is disrupted in other ways—by genetic mutation or chemical inhibition—this disruption also causes the genetic machinery to switch to the OFF phase, preventing further pilus formation.
"This was one of the big surprises," says Hultgren. "It's as if the bacteria senses that it has a non-functional adhesin and it switches off the whole pilus production assembly." This exposes a crucial weakness in this pathogen's ability to infect.
"Based on the mouse model, the crux of the whole infection cascade is the FimH attachment. If you don't have that, the bacteria can't stick to the bladder, invade, or cause infection," Hultgren notes. This means that drugs such as mannosides, chemical inhibitors that block FimH's attachment to cells, could work even more effectively by also keeping pilus gene expression switched off. Such drugs would block the bacteria from attaching and invading, so the body could simply flush them out in the urine flow.
Hultgren cautions that it will be a huge challenge to determine if the findings in the laboratory translate to human patients. But if so, Hultgren says, it would give drug developers a powerful, non-antibiotic way to fight UPEC: "FimH could be the Achilles' heel of UTIs."