Flow means 'go' for proper lymph system development
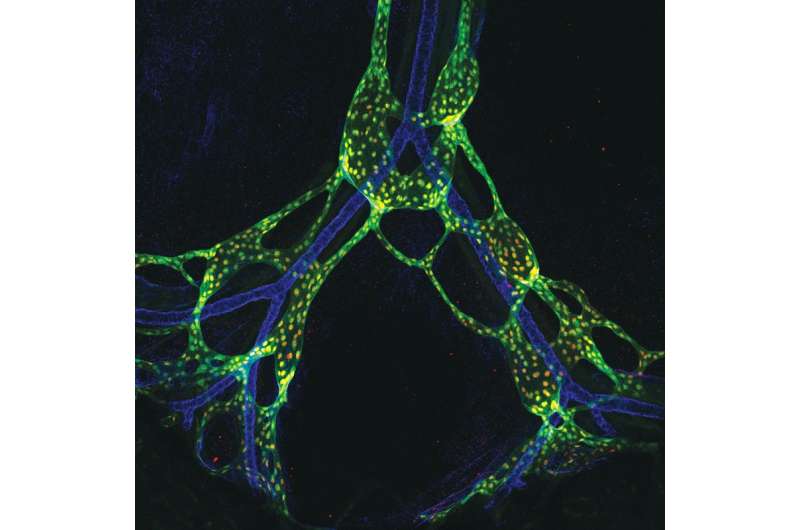
The lymphatic system provides a slow flow of fluid from our organs and tissues into the bloodstream. It returns fluid and proteins that leak from blood vessels, provides passage for immune and inflammatory cells from the tissues to the blood, and hosts key niches for immune cells. How this system develops hasn't been well understood, but now researchers from the Perelman School of Medicine at the University of Pennsylvania have found from experiments in mice that the early flow of lymph fluid is a critical factor in the development of mature lymphatic vessels.
"Once the primary lymph vessels are in place, an enormous amount of maturation has to happen, and what we've found is that the maturation process is triggered by physical forces from the earliest flow of lymph fluid in a developing embryo," said senior author Mark L. Kahn, MD, the Edward S. Cooper, M.D./Norman Roosevelt and Elizabeth Meriwether McLure Professor in the department of Medicine.
The findings, published online ahead of the August issue of the Journal of Clinical Investigation, represent a big step forward in the basic scientific understanding of lymphatic system development. They also should contribute to a better understanding of lymphatic disorders, including the lymphedema that affects many women following breast cancer surgery.
Mice With No Lymph Flow
The project was prompted in part by recent studies of cultured lymphatic vessel endothelial cells that suggested that fluid forces could be an important factor in the maturation of lymphatic vessels. But there was no straightforward way to test this hypothesis in live animals.
"No one had been able to come up with a way to stop lymph flow in embryonic animals, without preventing their lymphatic vessels from developing in the first place," said first author Daniel T. Sweet, PhD, a postdoctoral fellow in the Kahn Laboratory.
In humans and other mammals, the lymphatic system is a low-flow system that, unlike the blood circulatory system, has no central pump. Instead it relies on muscular contraction of the mature lymphatic vessel wall and small valves in lymphatic vessels to squeeze fluid along and prevent backflow.
Larger collecting lymphatic vessels receive many small inflows from lymphatic capillaries in surrounding tissues. "You can't just close one of the vessels to block flow downstream—there are many other tributaries coming in," said Sweet.
The solution to testing the role of flow in developing lymphatic vessels turned out to be a line of transgenic mice, developed earlier by the Kahn laboratory. Lacking a gene called Clec2, the mice fail to produce a certain receptor on blood platelets, with a remarkable result: veins that normally help drain the lymph system leak back into it. Like an ocean tide surging into a river, this upstream flow of blood stops the usual downstream flow of lymph.
Effects of No-flow
With fluorescent tracers, Sweet confirmed that the Clec2-knockout mice, as they developed, had no net flow of lymph. The animals did grow normal-looking primary network of lymphatic vessels, but as prior lab-dish studies had hinted might happen, those vessels failed to develop valves.
Unexpectedly, Sweet, Kahn and colleagues found that two other major features of the lymphatic system also failed to mature properly in these no-flow mice.
Normally after the initial phase of development of lymphatic vessels, a remodeling phase occurs in which the system makes itself more efficient. The vessels form a hierarchical structure in which smaller vessels upstream feed into larger vessels downstream. In the no-flow mice, this remodeling failed to occur.
What's more, the researchers found that smooth muscle cells, which normally form a thin lining in mature lymphatic vessels, and perform contractions that help lymph flow, instead formed an abnormally thick lining, as if the usual signal to shut off cell proliferation were missing.
"We started off thinking that flow might have a role just in valve formation, but ended up realizing that flow is really controlling all aspects of the maturation of these lymphatic vessels," said Sweet.
To demonstrate that these effects were due to the lack of lymph flow, not to a more direct impact of Clec2 deletion on lymphatic vessels, the researchers shut off Clec2 just in platelets, not in other cells, and saw the same results.
Cell culture studies, performed with Juan M. Jiminez, PhD, in the laboratory of collaborator Peter F. Davies, PhD, a professor of Pathology and Laboratory Medicine, also confirmed that the physical flow of fluid across lymphatic vessel cells could on its own stimulate gene expression changes closely resembling those known to direct lymphatic valve development.
Curiously, these cells appeared to need not just a forward movement of fluid, but at least a brief reversal, to stimulate gene expression changes. "It's like three steps forward, one step back, and we think that this flow-reversal is what induces the signaling," said Sweet.
The researchers now plan to study in more detail how lymphatic vessel cells turn the mechanical forces from lymph flow into the changes in gene expression needed for the maturation of lymphatic vessels. Another follow-on will be to investigate whether similar flow-related mechanisms drive the maturation of vessels and valves in the blood circulatory system.
Kahn expects that the research will also yield useful insights for treating lymphatic disorders, even those that occur in adults. One of the most common is the arm-swelling lymphedema that can follow the removal of armpit lymph nodes during breast cancer surgery. "We suspect that the flow of lymph works even after maturity, to maintain the appropriate molecular and genetic environment for these lymphatic vessels and valves," said Kahn. "Interrupting that flow might therefore have long-term adverse effects on those vessels and valves, so it raises the question of whether we need to restore the flow quickly at the time of lymph node removal."