Study compares combination treatments for black adults with asthma
Among black adults with asthma treated with an inhaled corticosteroid, adding a long-acting beta-agonist did not improve the time to an asthma exacerbation compared with adding the anticholinergic tiotropium, according to a study in the October 27 issue of JAMA.
National treatment recommendations suggest increasing inhaled corticosteroid (ICS) dose or adding a long-acting beta-agonist (LABA) to asthma patients with poor asthma control on low-dose ICS. However, asthma experts and the U.S. Food and Drug Administration have questioned the safety of LABA therapy, noting possible increases in serious events, including hospitalizations and death. Data suggest that LABA risks, if they exist, may disproportionately affect black populations and that black individuals may not benefit from LABAs to the same degree as individuals of other races. Investigations in predominantly white populations have attempted to determine if long-acting anticholinergics (a class of drugs that inhibit the transmission of certain nerve impulses, reducing spasms of smooth muscles, such as in the lungs) can substitute for LABAs in asthma, according to background information in the article.
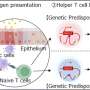
Michael E. Wechsler, M.D., M.Sc., of National Jewish Health, Denver, and Elliot Israel, M.D., of Brigham and Women's Hospital, Boston, and colleagues randomly assigned black adults with moderate to severe asthma to receive ICS plus either once-daily tiotropium (n = 532) or twice-daily LABAs (n = 538). Patients completed monthly questionnaires and were followed up for up to 18 months. Patients also underwent genetic testing. Some studies have suggested that a genetic variation may be associated with increased rates of adverse outcomes when LABAs are used for asthma, especially among black patients.
The researchers found that the primary outcome, time to first exacerbation, did not differ significantly between groups. In addition, LABA + ICS was not superior to tiotropium + ICS for secondary outcomes that addressed additional dimensions of asthma control, such as patient-reported outcomes (quality of life, asthma control, symptom index, symptom-free days), spirometry (a test of the air capacity of the lungs), rescue medication use, and asthma deteriorations.
Genetic variants were not associated with differential responses to therapy.
"These findings do not support the superiority of LABA + ICS compared with tiotropium + ICS for black patients with asthma," the authors write.
"Although we could not detect a difference in exacerbations between either combination therapy, we found that, despite combination therapy, this population experienced a high rate of exacerbations. Additional targeted interventions and further study are needed to reduce the rate of asthma exacerbations in this population."
More information: JAMA, DOI: 10.1001/jama.2015.13277