Study suggests new strategy for treating rare neurodegenerative disorder menkes disease
Treatments for Menkes disease, an inherited neurodegenerative disorder caused by a deficiency in copper, focus on delivering copper to the brain. The disease arises from dysfunction in ATP7A, a protein that transports copper to cells, and introducing working versions of the protein in the brain is considered the most direct therapeutic approach. However, a new study published in the American Physiological Society—Cell Physiology suggests that functioning ATP7A located elsewhere in the body, not necessarily the entire brain, can help treat the disorder.
Copper is essential for the structure and function of proteins that control the development of the central nervous system and other physiological processes. Infants born with Menkes disease show developmental issues, including brain abnormalities and intellectual disabilities. The development of hair, bones and arteries also depend on copper and are impaired in Menkes disease. Symptoms of the disorder include weakened bones, brittle hair and unusual skin and hair pigmentation.
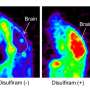
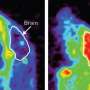
Administering copper to compensate for the copper deficiency does not work if ATP7A is completely dysfunctional. If ATP7A retains some function, patients show some neurodegeneration but copper administration can improve symptoms. To dissect the role of the body's transport of copper from the body's level of copper in central nervous system development, researchers at the University of Missouri created a mouse that was missing ATP7A only in cells of the central nervous system. Mice with defective ATP7A in every cell of the body, as occurs in the severe cases of Menkes disease, showed degenerated central nervous systems and died soon after birth. In comparison, the new mice had normal life spans and exhibited only mild neurological symptoms, including increased anxiety and greater susceptibility to seizures.
The study shows that the ATP7A gene is not required in the central nervous system of mice for viability, says lead researcher Michael Petris, PhD. The findings also suggest that to treat Menkes, "ATP7A function or expression may not need to be restored to the entire brain as a therapeutic strategy, for example by gene therapy. As long as copper entry to the central nervous system is achieved early in life, there may be significant improvement in disease progression," he says.
Scientists from the University of Nebraska—Lincoln and Marine Biological Laboratory also contributed to this study. The article "Autonomous requirements of the Menkes disease protein in the nervous system" is published in American Journal of Physiology—Cell Physiology.
More information: Victoria L. Hodgkinson et al. Autonomous requirements of the Menkes disease protein in the nervous system, American Journal of Physiology - Cell Physiology (2015). DOI: 10.1152/ajpcell.00130.2015