Critical immunotherapy target marks dysfunctional regulatory T cells in brain cancer
Immunotherapy represents an exciting advance in cancer treatment that harnesses the immune system to seek and destroy cancer cells. The programmed death 1 (PD-1) pathway dampens immune responses to tumor cells, and several clinical trials have shown favorable outcomes by targeting PD-1 or its ligand PD-1L.
In this issue of JCI Insight, David Hafler and colleagues at Yale University and Massachusetts Institute of Technology examined PD-1-expressing regulatory T cells in glioblastoma multiforme, an extremely aggressive form of brain cancer. Regulatory T cells normally constrain immune responses and keep other types of T cells from mounting hyper-aggressive responses.
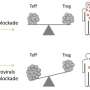
Although anti-PD1 therapy is generally thought to promote conventional T cell activity, the Hafler team now reports that PD-1 expression on regulatory T cells from the tumors of glioblastoma multiforme patients correlates with regulatory T cell dysfunction.
They also found that glioblastoma multiforme patients treated with a PD-1 blocking antibody had a higher proportion of dysfunctional regulatory T cells. These observations suggest the possibility that PD-1 targeting therapies could work, in part, by driving further regulatory T cell dysfunction.
Future studies will be needed to more fully understand the contribution of this pathway to anti-tumor effects.
More information: Daniel E. Lowther et al, PD-1 marks dysfunctional regulatory T cells in malignant gliomas, JCI Insight (2016). DOI: 10.1172/jci.insight.85935