Enzyme in myelination process could lead to better understanding of neurological disorders
The removal of the enzyme Dnmt1 during oligodendrocyte progenitor cell (OPC) differentiation in the central nervous system resulted in inefficient myelin formation and neurological deterioration, including loss of control of bodily movements, in mice, according to a study conducted at the Icahn School of Medicine at Mount Sinai and published today in the medical journal Cell Reports. The results could lead to a new understanding of multiple sclerosis and other myelin disorders in humans.
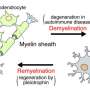
Oligodendrocytes (OLs) are cells with the ability to form a specialized membrane that is called "myelin." Myelin is the insulating sheathing around the axons of nerve cells, which provides energetic support and allows for faster electrical impulse conduction. OLs are derived from progenitors called OPCs, which are stem-like cells with the ability to divide and generate OLs through a complex process of gene regulation.
This study shows that the development of OPCs into myelin-forming cells requires DNA methylation, which is a process consisting of the addition of chemical groups to the DNA carried out by enzymes called methyl transferases (DNMTs). When these groups are added, genes cannot be expressed and therefore are "silenced." The authors identify the many genes needed to be "silenced" in OPCs in order to allow for proper formation of myelin during development.
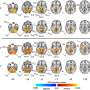
Researchers showed that the removal of Dnmt1 in oligodendrocyte lineage not only limited cell growth, but also led to cellular stress as well as severe and clinically symptomatic hypomelination - a reduced amount of myelin in nervous tissue. The mice experienced significant neurological symptoms, such as tremors and a loss of control of body movement, and eventually death.
"Our group has previously observed altered DNA methylation in the brain of patients with multiple sclerosis, the most devastating adult demyelinating disorder, but its role in myelin formation and the identity of the genes silenced by DNMT's in OPCs were not known," says lead investigator Patrizia Casaccia, MD, PhD, Professor of Neuroscience, Genetics and Genomics, and Neurology, and Chief of the Center of Excellence for Myelin Repair at the Friedman Brain Institute at the Icahn School of Medicine. "A better understanding of why DNA methylation is important for myelin formation and what genes need to be shut off during the formation of OLs from OPCs has important implications not only for development, but also for myelin repair."
The research could lead to the development of treatment for disorders where the myelin sheath is damaged and could also help in understanding how OPCs transform into brain cancer cells.
Further study is needed to understand the causes underlying aberrant DNA methylation in the brains of multiple sclerosis patients and in preclinical models. Translational applications will include the identification of factors that could bypass impaired DNA methylation.