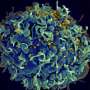
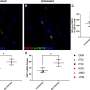
New research explains why HIV is not cleared by the immune system
Scientists at the University of North Carolina (UNC) School of Medicine and Sanford Burnham Prebys Medical Discovery Institute (SBP) have identified a human (host) protein that weakens the immune response to HIV and other viruses. The findings, published today in Cell Host & Microbe, have important implications for improving HIV antiviral therapies, creating effective viral vaccines, and advance a new approach to treat cancer.
"Our study provides critical insight on a paramount issue in HIV research: Why is the body unable to mount an efficient immune response to HIV to prevent transmission?" said Sumit Chanda, Ph.D., professor and director of SBP's Immunity and Pathogenesis Program and co-senior author of the study. "This research shows that the host protein NLRX1 is responsible—it's required for HIV infection and works by repressing the innate immune response."
The innate immune response works by producing a cascade of signaling chemicals (interferons and cytokines) that trigger cytotoxic T cells to kill pathogens. Increasing evidence suggests that mounting an early, potent innate immune response is essential for the control of HIV infection, and may improve the effectiveness of vaccines.
"Importantly, we were able to show that deficiencies in NLRX1 reduce HIV replication, suggesting that the development of small molecules to modulate the innate immune response may inhibit viral transmission and promote immunity to infection," said Chanda. "We anticipate expanding our research to identify NLRX1 inhibitors."
How NLRX1 reduces innate immunity to HIV
Although HIV is a single-stranded RNA virus, after it infects an immune cell it's rapidly reverse transcribed into DNA, increasing the level of DNA found in the fluid portion of a cell (cytosol). Elevated cytosolic DNA triggers a sensor called STING (stimulator of interferon genes) that turns on the innate immune response.
"Until now, the mechanism by which NLRX1 promoted HIV infection was unexplored. We have shown that NLRX1 interacts directly with STING, essentially blocking its ability to interact with an enzyme called TANK-binding kinase 1 (TBK1)," said Haitao Guo, Ph.D., senior postdoctoral research associate in the laboratory of Jenny Ting, Ph.D., a University of North Carolina Lineberger Comprehensive Cancer Center member, the William R. Kenan Jr. Professor of Microbiology and Immunology at the UNC School of Medicine and lead author of the study. "The STING-TBK1 interaction is a critical step for interferon production in response to elevated cytosolic DNA, and initiates the innate immune response."
"This research expands our understanding of the role of host proteins in viral replication and the innate immune response to HIV infection, and can be extended to DNA viruses such as HSV and vaccinia," added Guo.
Relevance to cancer
"Our discovery that NLRX1 reduces the immune response to HIV is similar to the discovery of host immune checkpoints, such as PD-L1 and CTLA-1, that control the immune response to cancer," said Ting, co-senior author of the study.
Immune checkpoints are immunological "brakes" that prevent the over-activation of the immune system on healthy cells. Tumor cells often take advantage of these checkpoints to escape detection of the immune system. Several FDA-approved drugs that target checkpoints, called checkpoint inhibitors, are now available to treat certain cancers.
"Checkpoint inhibitors have made a huge impact on cancer treatment, and significant investment by the biotech/pharmaceutical sector is being made to identify STING inhibitors as the next generation of immune-oncology therapeutics," said Ting. "This study, showing that NLRX1 is a checkpoint of STING, sheds more light on the topic and will help advance those efforts."
More information: Haitao Guo et al. NLRX1 Sequesters STING to Negatively Regulate the Interferon Response, Thereby Facilitating the Replication of HIV-1 and DNA Viruses, Cell Host & Microbe (2016). DOI: 10.1016/j.chom.2016.03.001