Scientists solve immune system mystery for Type 1 diabetes
Scientists have solved a decades-old medical mystery by finally identifying a previously unknown molecule which is attacked by the immune system in people with Type 1 diabetes.
The ground-breaking research, led by Dr Michael Christie from the University of Lincoln, UK, could now lead to better identification of individuals at risk of Type 1 diabetes and inform the development of new therapies which could prevent the disease developing.
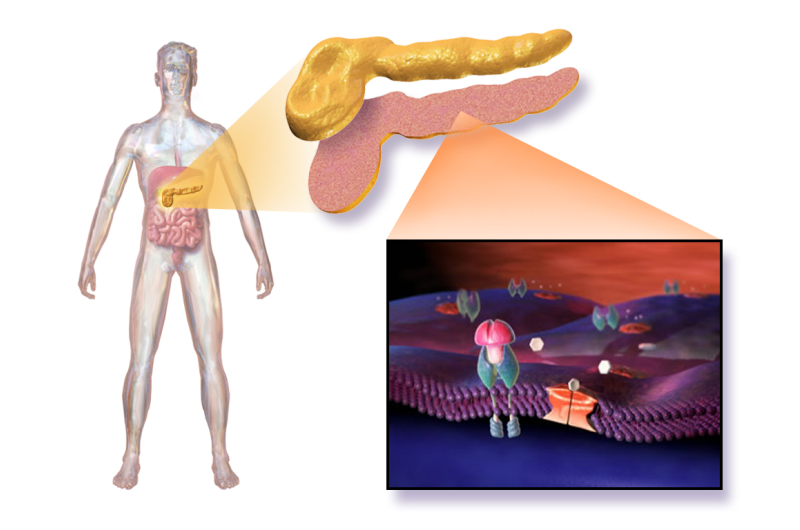
Type 1 diabetes develops when the body is unable to produce insulin; a substance required to regulate blood sugar levels by moving glucose out of the blood and into cells to be used for energy. It is an autoimmune disease, where the body's defence system that normally protects against infections attacks and destroys the insulin-producing cells in the pancreas.
In Type 1 diabetes, the immune system reacts to particular molecules in the pancreas – called autoantigens - that it would normally ignore. People with Type 1 diabetes have antibodies in their blood that are specific to each of the molecules. Tests are currently used to detect these antibodies: the more antibodies detected, the higher the risk a person has of developing Type 1 diabetes. The tests are currently used to identify those most at risk of Type 1 diabetes, and in the future could provide an opportunity to intervene and stop the disease in its tracks.
Until now, scientists had found four molecules that are attacked by the immune system in Type 1 diabetes. The identity of a fifth molecule – known only as 'Glima' for the past 20 years – has been a mystery. Dr Christie's team have successfully identified this fifth molecule as Tetraspanin-7, which could make tests for predicting Type 1 diabetes more accurate. They are now searching for ways to block the immune attack, in order to prevent Type 1 diabetes from developing in those at a high risk.
The research was funded by Diabetes UK and the Society for Endocrinology and is published in Diabetes, the journal of the American Diabetes Association.
Dr Christie, Reader in the School of Life Sciences at the University of Lincoln, said: "Being able to detect circulating autoantibodies and identify their molecular targets has allowed scientists to develop tests for the clinical diagnosis of Type 1 diabetes, and for the identification of individuals at high risk of developing the disease. Evidence from both animal studies and human trials indicate that Type 1 diabetes may be prevented in individuals at risk, and a number of therapies to interfere with immune responses have proved effective in preventing disease development in animals and in slowing the loss of insulin-secreting cell function in human patients.
"There is now a focus on the development of procedures to interfere specifically in immune responses that cause Type 1 diabetes, and it is therefore absolutely essential that we gather as much information as possible about the major targets of autoimmune responses.
"We already had some knowledge about the physical properties of 'Glima' but its molecular identity has for many years proved elusive. This has hampered the development of relevant autoantibody tests, but our research successfully identified 'Glima' as the substance Tetraspanin-7. We can now exploit this knowledge for diabetes prediction and immunotherapy."
Screening for antibodies against the four molecules found in the pancreas is currently used to assess a person's risk of Type 1 diabetes. Following Dr Christie's research, Tetraspanin-7 antibodies could now be included in this process. This could make tests more accurate and help researchers to understand a person's individual and unique immune response – both of which are crucial in the development of treatments that can stop the progression of Type 1 diabetes.
A member of the research team, Dr Kerry McLaughlin, has been awarded a fellowship by the charity JDRF to develop new tests to detect Tetraspanin-7's antibodies and better understand its function at the University of Oxford.
Dr Emily Burns, Research Communications Manager at Diabetes UK, said, "In order to prevent Type 1 diabetes, we need to fully understand how the immune response that damages insulin-producing cells develops in the first place. Dr Christie's impressive research is helping us to do just that. We hope that the findings here will be used to improve the identification of those at risk of Type 1 diabetes and, in the long-term, inform the crucial development of therapies that can stop this immune response from happening and ultimately prevent Type 1 diabetes."
More information: Kerry A. McLaughlin et al. Identification of Tetraspanin-7 as a Target of Autoantibodies in Type 1 Diabetes, Diabetes (2016). DOI: 10.2337/db15-1058