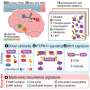
Next-generation gene sequencing helps diagnose rare diseases in newborns
The use of next-generation gene sequencing in newborns in neonatal intensive care units (NICUs) may improve the diagnosis of rare diseases and deliver results more quickly to anxious families, according to new research in CMAJ (Canadian Medical Association Journal).
"Next-generation sequencing has the potential to transform the practice of clinical genetics rapidly," writes Dr. David Dyment, Children's Hospital of Eastern Ontario (CHEO), with coauthors. "In particular, newborns admitted to the NICU with rare and complex diseases may benefit substantially from a timely molecular diagnosis through next-generation sequencing."
Children with suspected rare genetic diseases usually undergo a battery of tests to determine a molecular diagnosis. Current practice involves testing of specific genes or a panel of genes, and these tests are often done outside the country because of limited availability within Canada. This means it may be months or even years before a diagnosis is made.
There are few studies to date looking at the feasibility and diagnostic success rate of next-generation sequencing in the NICU.
Canadian researchers conducted a pilot study with 20 newborns to determine the effectiveness of a targeted next-generation sequencing panel that included all 4813 genes currently known to be associated with rare diseases. The 20 newborns presented with a wide range of complex, medical issues, and half had neurologic symptoms such as seizures or hypotonia. Next-generation sequencing provided a molecular diagnosis for 40%, or 8 of the 20 infants. In two of the infants, the molecular diagnoses had a direct impact on their medical management.
"This technique can be performed in a hospital-based laboratory without the need to send samples away, often out of the country," states Dr. Dyment. "This will allow for diagnoses to be made quickly, providing answers to anxious families and potentially life-saving interventions in some cases."
The researchers suggest that adopting this type of technology in Canadian hospitals will greatly increase the ability to diagnose rare diseases and treat children while saving health care dollars.
"Enabling the family to understand why their baby is ill can help to assuage the almost universal guilt felt by parents that they did something wrong to cause their baby's illness," writes Dr. Sarah Bowdin, Clinical and Metabolic Genetics, Hospital for Sick Children (SickKids), Toronto, Ontario, in a related commentary. "It can also indicate whether other family members may be at risk of the same disease and provide an accurate recurrence risk for future pregnancies."
Building strong partnerships with specialists such as neonatologists, intensive care physicians and genetics laboratories is critical to ensure the success of this diagnostic tool.
More information: CMAJ paper: www.cmaj.ca/lookup/doi/10.1503/cmaj.150823
Commentary: www.cmaj.ca/lookup/doi/10.1503/cmaj.160490