Persistent depression linked to increased CAC scores in women
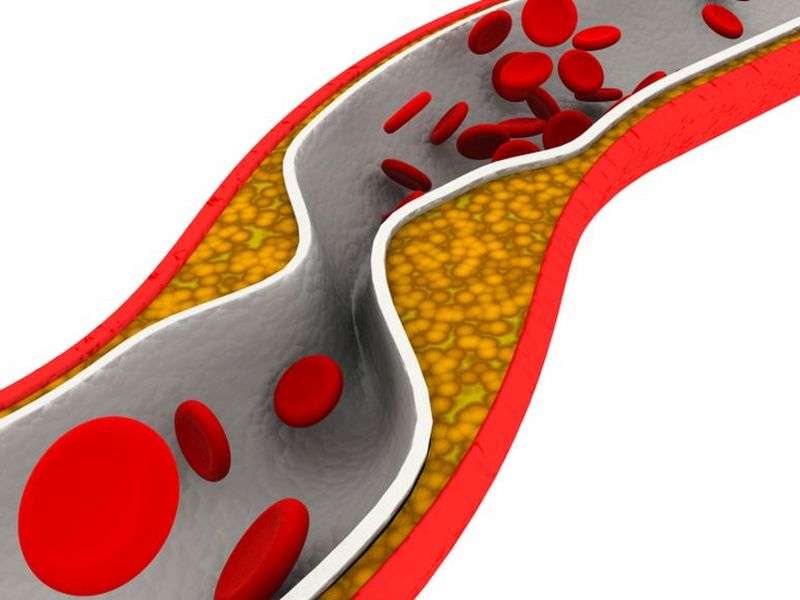
(HealthDay)—Persistent depressive symptoms are associated with increased coronary artery calcium (CAC) scores among middle-aged women without cardiovascular disease (CVD), according to a study published in the June 15 issue of The American Journal of Cardiology.
Imke Janssen, Ph.D., from the Rush University Medical Center in Chicago, and colleagues assessed participants in the Study of Women's Health Across the Nation Heart study annually for depressive symptoms over five years before CAC assessment.
The researchers found that high depressive symptoms were common over five years in middle-aged women free from CVD and diabetes: 19 percent had one, 9 percent had two, and 11 percent experienced three or more episodes. Overall, CAC was low, with 54, 25, and 21 percent having no CAC, 0 to 10, and ≥10 Agatston units, respectively. Compared to women with no depressive episodes, women with three or more episodes were twice as likely to have significant CAC (≥10 Agatston units), after adjustment for CVD risk factors (odds ratio, 2.20), with no difference by race. There was no difference for women with one or two episodes versus no episodes.
"In healthy women aged 46 to 59 years without clinical CVD or diabetes, persistent depressive symptoms were significantly associated with elevated CAC scores, suggesting that they are more likely to have pathophysiological and behavioral effects on the development of subclinical CVD than does a single episode of elevated depressive symptoms," the authors write.
More information:
Abstract
Full Text (subscription or payment may be required)
Copyright © 2016 HealthDay. All rights reserved.