Not all sleep apnea patients are obese
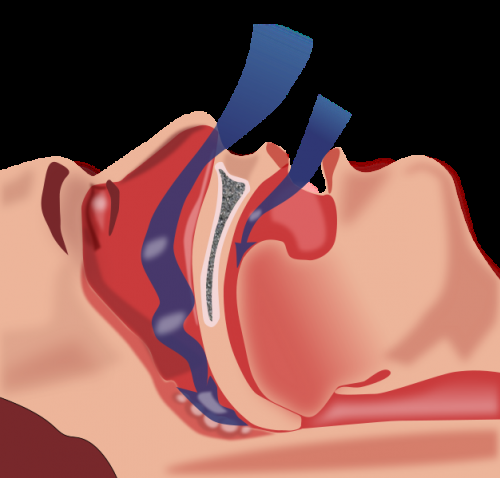
Contrary to popular opinion, not all people who suffer from obstructive sleep apnea (OSA) are obese. However, a new study from Neuroscience Research Australia (NeuRA) and the Prince of Wales Hospital (POWH) highlights that normal-to-overweight patients with OSA likely require a different approach to treatment, which presents a challenge to clinicians.
Obstructive sleep apnoea, a common condition that affects more than one million Australians, occurs when the throat closes off many times throughout the night – up to 100 times per hour of sleep – which limits breathing during the night.
Obesity can cause an anatomical obstruction of the upper airway and is a well-established risk factor for sleep apnea. However, more than half the population referred to the POWH Sleep Clinic for suspected OSA was not obese.
This is the first study to highlight that respiratory arousal, a key contributor to OSA that is not related to anatomy, differs in non-obese versus obese patients. The latter population responds well to continuous positive airway pressure (CPAP) treatment, but this is not the case with normal-to-overweight patients.
The study found that the majority of non-obese patients suffer from a low respiratory arousal threshold, which means they have a greater tendency to wake easily. This may be a factor that limits their tolerance for CPAP therapy.
"Non-obese OSA patients are a challenging group to treat with existing therapies as they are less adherent and compliant with CPAP therapy compared to obese patients with sleep apnea," says study author Assoc Prof Danny Eckert.
Accordingly, clinicians need to keep BMI in mind when prescribing therapies for patients. "Specifically, they may need therapies that target causes other than upper airway anatomy such as sleep promotion aids to allow for deeper more stable sleep and breathing," says Assoc Prof Eckert. "Or they could use these approaches in combination with the CPAP for greater therapeutic advantage. This also means that doctors and clinicians need to look for other symptoms associated with OSA when patients present with sleeping issues beyond obesity and anatomical issues".
Assoc Prof Eckert reiterated that CPAP remains the first-line treatment recommendation, regardless of BMI, but that more research was required to better understand the treatment needs for non-obese patients.
This study will be published in the Journal of Clinical Sleep Medicine.
More information: Obstructive Sleep Apnea Without Obesity is Common and Difficult to Treat: Evidence for a Distinct Pathophysiological Phenotype. J Clin Sleep Med. 2016 Sep 13. pii: jc-00147-16. [Epub ahead of print] www.ncbi.nlm.nih.gov/pubmed/27655455