Corneal transplantation may improve outcomes in people with a degenerative eye disease
An innovative procedure may improve outcomes in people with a degenerative eye disease, suggest five-year results from a study presented at AAO 2016, the 120th annual meeting of the American Academy of Ophthalmology. Transplantation of one layer of the cornea may help people with keratoconus avoid or delay full corneal transplantation and other potentially risky procedures, according to the researchers. They say the technique may enable those with advanced keratoconus to tolerate extended contact lenses wear, which is traditionally a challenge for people with the condition.
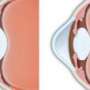
Keratoconus is a disease that causes the cornea - the clear front of the eye - to thin and become cone-shaped. Symptoms often first appear in childhood or the teen years. The disease only effects one in 2,000 people, but it can lead to severe visual impairment. Traditional treatment options, including corneal transplantation, are limited or risky due to the complexity of the disease. In addition, keratoconus patients are unable to wear contact lenses for an extended time to correct vision due to their cone-shaped corneas. To address these issue, researchers in the Netherlands sought to study whether only transplanting the second layer of the cornea - the Bowman layer - would be a safe and effective alternative to full corneal transplantation in the long term. They also hoped the procedure would enable patients to wear contact lenses. After providing the treatment to 19 patients and following them for 5 years, the researchers determined the treatment improved recipients' vision and stabilized the disease in 90 percent of the eyes.
Currently, there are four common treatments for keratoconus. In its early stages, the condition can be treated using glasses or contact lenses. As the condition progresses, glasses may no longer work and many people are unable to wear contact lenses because the lenses no longer fit as the corneas become more cone-shaped. Another treatment uses a laser and eyedrops to promote strengthening of the collagen fibers that make up the cornea, a procedure called cross-linking. A third option is a procedure called Deep Anterior Lamellar Keratoplasty, or DALK, which involves implantation of the front and middle layers of the cornea. Ultimately, some people require a full corneal transplantation to restore their vision, which involves removing the damaged cornea and replacing it with one from a donor. Complications of the various corneal transplants include wound healing difficulties and persistent astigmatism, which causes distorted vision.
The innovative technique used in the study involves placing donor tissue from the second layer of the cornea - the Bowman layer - into the middle layer through a tiny tube. This strengthens and flattens the cornea, improving vision. The Bowman layer is ideal for transplantation because it does not contain cells. The body often rejects cell-containing tissue transplanted from another person because it perceives the tissue as foreign and potentially dangerous. Placing it in the middle layer of the corner appears to prompt the healing response, researchers said. Because it doesn't involve cutting or stitching, it is less risky than some procedures to treat keratoconus, including full corneal transplantation.
Researchers at the Rotterdam, Netherlands Institute for Innovative Ocular Surgery, Melles Cornea Clinic and Amnitrans Eye Bank transplanted the Bowman layer in 22 eyes in 19 people with advanced keratoconus. These patients were not candidates for corneal cross-linking because their corneas were too steep and thin. They were also unable to wear contact lenses for an extended time, and had 20/400 vision while wearing glasses.
Following the procedure, the results were as follows:
- Disease progression was halted in 20 of the eyes, or 90 percent, which is the main goal of the treatment.
- The patients' corrected vision improved to 20/200.
- All the patients could tolerate extended contact lens wear. The average best-corrected vision with contact lenses held stable at 20/40 from pre- to postoperatively.
None had postoperative complications that can occur with corneal transplantation, such as wound healing difficulties and persistent astigmatism, which causes distorted vision.
"Bowman layer transplantation may be safer than a full corneal transplant, is effective and the benefits last," said Jack Parker, M.D., lead author of the study and a corneal fellow at the Netherlands Institute for Innovative Ocular Surgery. "The procedure can spare young people with the condition a lifetime of difficult, expensive and risky eye procedures and interventions."
The limitations of the study are a relatively small study population and no control group. Researchers say the technique should be studied in a larger group.