Pediatric tuberculosis in Canada: A guide for physicians
Although pediatric tuberculosis (TB) remains relatively uncommon in Canada, some populations—including Aboriginal communities—have a much higher burden of disease. As a result, Canada should focus on addressing the high rates of the disease in these communities, according to a review in CMAJ (Canadian Medical Association Journal).
Children who have immigrated to Canada from countries with endemic TB, and those whose parents have come from these countries, are also at higher risk.
"High rates of TB among the Inuit and other Aboriginal groups in Canada deserve much greater national focus and will require coordinated public health measures and innovative programs but also substantial improvement in housing and living conditions," writes Dr. Ian Kitai, The Hospital for Sick Children (SickKids), Toronto, Ontario, with coauthors.
The overall rate of TB in Canada is 4.4 per 100 000 people, but in Nunavut, the estimated rate is 227 per 100 000, one of the highest known rates of TB worldwide.
The article reviews the symptoms, diagnostic testing of children with TB in Canada, safe management of latent infection and the epidemiology of the disease.
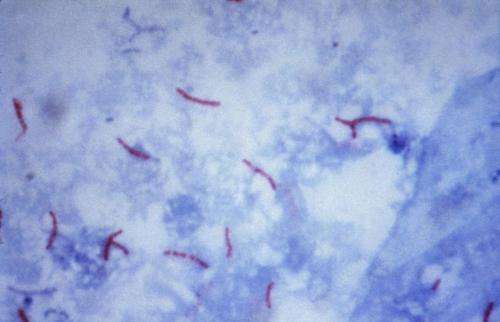
Symptoms of TB in older children and adolescents include prolonged fever, weight loss and night sweats. Those with lung disease may have cough with mucus (which may sometimes be bloody) and organs other than the lungs are often affected as well. Younger children and infants often present with non-specific symptoms. As TB can masquerade as other diseases, diagnostic testing and clinical suspicion are important for diagnosis. Testing includes chest radiographs, microbiologic tests of sputum and biopsy of other affected organs. TB skin tests and interferon gamma release assays aid diagnosis but may be negative in some patients with TB disease. These tests also help identify those with latent ("sleeping") infection who are at risk for developing active TB disease.
"Because of the myriad ways in which TB can present, TB disease should be suspected in any child with epidemiologic risk factors and suggestive symptoms or signs of organ involvement that are not explained by other diagnoses," the authors write. "Clinical suspicion is critical."
Treatment, which includes multiple drugs, is most effective when delivered by a team made up of clinicians, public health nurses, translation services in case of language difficulties and social workers with experience in managing pediatric TB.
Screening and treatment of those at risk for latent TB infection, early diagnosis of tuberculosis disease, and monitoring of medication can help prevent the spread of TB. Tuberculosis elimination in Canada also requires strong public health infrastructure and improvement in social determinants of health locally, and will be aided by Canada's participation in international efforts to reduce the global TB epidemic.
More information: Canadian Medical Association Journal, www.cmaj.ca/lookup/doi/10.1503/cmaj.151212