October 20, 2015 report
DNA analysis shows that tuberculosis in northern Canada started with white settlements
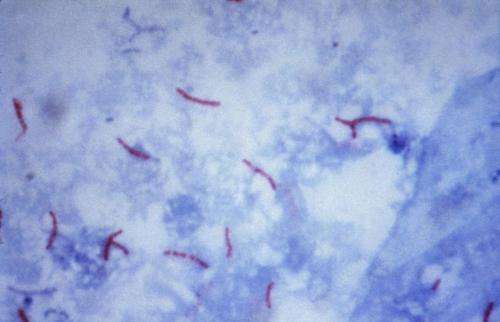
(Medical Xpress)—A team of academic and governmental researchers in Canada has found that the ongoing tuberculosis epidemic in northern Canada got its start back in the early 1900's when the first white settlements were established. In their paper published in Proceedings of the National Academy of Sciences, the team describes their genetic study of strains of the disease found in several Inuit areas and what was revealed.
Several parts of northern Canada are experiencing an ongoing tuberculosis epidemic among native Inuit people—Nunavik, Québec is one example, with infection rates fifty times as high as in the southern part of the country. And while the reasons for the continuation of the spread of the disease are clear (poverty and people living in close quarters) the history of the disease in Canada has not been so obvious. To learn more about the disease, to help stop its spread, the researchers with this new effort collected samples from infected people in many heavily impacted settlements and conducted a DNA analysis—the goal was to determine if there was just one major strain and whether it was resistant.
Tuberculosis is mainly a disease of the lungs, though most who are infected never realize that it has occurred—it is only when the bacteria responsible for it overcome the immune system that it becomes problematic. Global health experts estimate that one in three people alive today carry the bacteria around inside of them, most in Asia. When it goes active, symptoms generally include coughing up blood, fever and weight loss (the origin of the old name for the disease—consumption).
In all, the researchers collected samples from 163 people and discovered that the majority of cases were due to the Mycobacterium tuberculosis strain, which was actually good news—it is the most prevalent strain in the world and is not considered resistant to treatment drugs. They were also able to trace the introduction of the disease back to approximately 1919—a time when white settlers first began setting up trading posts and other permanent settlements in place that had been exclusively Inuit.
The findings by the team confirm suspicions that the persistence of the disease in northern Canada is due primarily to social conditions, which means that given the right attention, it should be controllable.
More information: Population genomics of Mycobacterium tuberculosis in the Inuit, Robyn S. Lee, DOI: 10.1073/pnas.1507071112
Abstract
Nunavik, Québec suffers from epidemic tuberculosis (TB), with an incidence 50-fold higher than the Canadian average. Molecular studies in this region have documented limited bacterial genetic diversity among Mycobacterium tuberculosis isolates, consistent with a founder strain and/or ongoing spread. We have used whole-genome sequencing on 163 M. tuberculosis isolates from 11 geographically isolated villages to provide a high-resolution portrait of bacterial genetic diversity in this setting. All isolates were lineage 4 (Euro-American), with two sublineages present (major, n = 153; minor, n = 10). Among major sublineage isolates, there was a median of 46 pairwise single-nucleotide polymorphisms (SNPs), and the most recent common ancestor (MRCA) was in the early 20th century. Pairs of isolates within a village had significantly fewer SNPs than pairs from different villages (median: 6 vs. 47, P < 0.00005), indicating that most transmission occurs within villages. There was an excess of nonsynonymous SNPs after the diversification of M. tuberculosis within Nunavik: The ratio of nonsynonymous to synonymous substitution rates (dN/dS) was 0.534 before the MRCA but 0.777 subsequently (P = 0.010). Nonsynonymous SNPs were detected across all gene categories, arguing against positive selection and toward genetic drift with relaxation of purifying selection. Supporting the latter possibility, 28 genes were partially or completely deleted since the MRCA, including genes previously reported to be essential for M. tuberculosis growth. Our findings indicate that the epidemiologic success of M. tuberculosis in this region is more likely due to an environment conducive to TB transmission than a particularly well-adapted strain.
© 2015 Medical Xpress