Effort to reduce 'covert' brain injury after cardiac procedures
Patients who undergo lifesaving cardiac procedures are often exposed to a related harm: brain injury. In response to a growing body of evidence of this problem, Yale professor of medicine Dr. Alexandra Lansky joined colleagues in the United States and Europe to call for measures to better ensure the safety of cardiac procedures.
During certain cardiac procedures, patients are at risk for strokes due to the release of emboli, or particulate material such as a plaque, that travel in the blood from the heart to the brain.
"As even the smallest damage to particular parts of the brain can impact a patient's memory and day-to-day ability to function, my colleagues and I have grown increasingly concerned that safety evaluations of the newer cardiovascular procedures only evaluate the extreme life-threatening forms of brain damage," said Lansky, co-chair of The Neurologic Academic Research Consortium, which produced the paper.
"This paper outlines the need to use and report more modern and sensitive measures to evaluate brain injury related to cardiac procedures," she said.
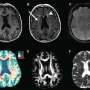
Strokes are among the most feared and costly complications of cardiovascular interventions and are under-reported in clinical trials, note the researchers. To address the issue, in the paper, Lansky and her colleagues offer a simple classification of the levels of potential damage to the brain, including overt damage such as stroke; covert injury recognized by brain imaging; and neurologic dysfunction, which encompasses a range of symptoms not visible in brain imaging.
More information: Alexandra J. Lansky et al. Proposed Standardized Neurological Endpoints for Cardiovascular Clinical Trials, Journal of the American College of Cardiology (2017). DOI: 10.1016/j.jacc.2016.11.045