Hair testing shows high prevalence of new psychoactive substance use
In the last decade hundreds of new psychoactive substances (NPS) have emerged in the drug market, taking advantage of the delay occurring between their introduction into the market and their legal ban. According to the Drug Enforcement Agency (DEA) NPS describes a recently emerged drug that may pose a public health threat. The DEA issues a quarterly Emerging Threat Report, which catalogues the newest identified NPS.
NPS tend to mimic the psychotropic effects of traditional drugs of abuse, but their acute and chronic toxicity, and side-effects are largely unknown. While seizure data from the DEA is often used to indicate what new drugs are being sold in the US, there is a lack of research examining and confirming who has been using such drugs.
Joseph J. Palamar, PhD, MPH, a New York University researcher, has been researching incidental and intentional use of NPS by young adults. His current line of inquiry has focused on survey methods, qualitative interviews, and hair sampling to ascertain frequency and type of NPS use by nightclub-goers—a demographic which traditionally has a relaxed view towards recreational drug experimentation and use.
NPS are common adulterants in drugs such as ecstasy (MDMA), which has seen an increase in popularity since it became marketed as "Molly". Ironically, "Molly" connotes a product that is pure MDMA. In a related study, Palamar and his team found that four out of ten nightclub/festival attendees who used ecstasy or "Molly" tested positive for "bath salts" despite reporting no use.
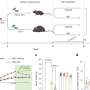
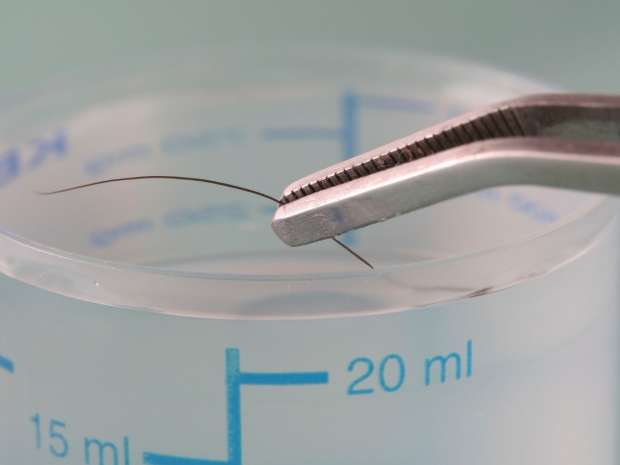
In their current study, "Hair Testing for Drugs of Abuse and New Psychoactive Substances in a High-Risk Population," Dr. Alberto Salomone, an affiliated researcher at the Centro Regionale Antidoping e di Tossicologia "A. Bertinaria", Orbassano, Turin, Italy and Dr. Palamar, affiliated with NYU's Center for Drug Use and HIV Research (CDUHR), collected hair samples from 80 young adults outside of New York City nightclubs and dance festivals, from July through September of 2015. Hair samples from high-risk nightclub and dance music attendees were tested for 82 drugs and metabolites (including NPS) using ultra-high performance liquid chromatography-tandem mass spectrometry.
"Hair analysis represents a reliable and well-established means of clinical and forensic investigations to evaluate drug exposure, said Dr. Salomone. "Hair is the most helpful specimen when either long-time retrospective information on drug consumption is of interest." "Most NPS can no longer be detected in urine, blood, or saliva within hours or days after consumption, but hair is particularly beneficial because many drugs can be detected months after use."
Of the eighty samples, twenty-six tested positive for at least one NPS—the most common being a "bath salt" (synthetic cathinone) called butylone (present in twenty-five samples). The "bath salts" methylone and even alpha-PVP (a.k.a.: "Flakka") were also detected. The researchers find the presence of Flakka alarming as this drug has been associated with many episodes of erratic behavior and even death in Florida. Other new drugs detected included new stimulants called 4-FA and 5/6-APB.
"We found that many people in the nightclub and festival scene have been using new drugs and our previous research has found that many of these people have been using unknowingly," said Dr. Palamar, also an assistant professor of Population Health at NYU Langone Medical Center (NYULMC).
Hair analysis proved a powerful tool to Drs. Salomone and Palamar and their team, allowing them to gain objective biological drug-prevalence information, free from possible biases of unintentional or unknown intake and untruthful reporting of use.
"Such testing can be used actively or retrospectively to validate survey responses and inform research on consumption patterns," notes Dr. Palamar.
The full results of the present study can be found in the Journal of Analytical Toxicology.
More information: Alberto Salomone et al. Hair Testing for Drugs of Abuse and New Psychoactive Substances in a High-Risk Population, Journal of Analytical Toxicology (2017). DOI: 10.1093/jat/bkx020