Mapping IDs geographic access barriers for diabetic retinopathy

(HealthDay)—Geographic information systems mapping can visualize geographic access barriers to eye care among patients with diabetes, while telescreening can increase the rate of diabetes retinopathy evaluation, according to two studies published online May 18 in JAMA Ophthalmology.
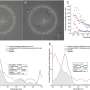
Pooja D. Jani, M.D., from the University of North Carolina at Chapel Hill, and colleagues used geographic information systems mapping techniques to visualize access barriers to eye care for patients with diabetes in a cross-sectional study conducted in five primary care clinics in North Carolina. A total of 1,787 patients with diabetes received retinal screening photographs with remote expert interpretation to identify diabetic retinopathy. The researchers found that the widest distribution of zip codes was seen at the Greenville site. Ophthalmologists were concentrated around urban centers, while primary care physicians were spread across the state.
In a second study, Jani and colleagues examined retinal telescreening for patients with diabetes in a pre- and postimplementation evaluation. Data were included for 1,661 patients at five primary care clinics serving rural and underserved populations in North Carolina. The researchers found that the mean rate of diabetic retinopathy screening was 25.6 percent before implementation of the program, and increased to 40.4 percent after implementation. Within the study period, 60 percent of referred patients completed an ophthalmology referral visit. The odds of requiring a referral were increased for older patients, African-American patients, and other racial/ethnic minorities (odds ratios, 1.28, 1.84, and 2.19).
"Retinal telescreening increased the rate of evaluation for DR for patients in rural and underserved settings," the authors write in the second study.
One author from both studies disclosed financial ties to Welch Allyn.
More information:
Abstract/Full Text 1 (subscription or payment may be required)
Abstract/Full Text 2 (subscription or payment may be required)
Editorial (subscription or payment may be required)
Copyright © 2017 HealthDay. All rights reserved.