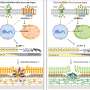
Photoreceptor cell death leads to blindness in CLN5 form of Neuronal Ceroid Lipofuscinosis
Researchers from the University of Eastern Finland have discovered a likely cause for visual impairment and eventual loss of vision in the Finnish variant of Neuronal Ceroid Lipofuscinosis (NCL). Visual impairment associated with the Finnish variant of NCL may be caused by impaired retinal waste management system, including autophagy, leading primarily to the death of photoreceptor cells that are of essential for vision.
The NCLs are the most common neurodegenerative disease group among children. NCL diseases constitute part of the Finnish disease heritage and they are more common in Finland than anywhere else in the world. Childhood NCL diseases lead to loss of vision and to premature death. No drug therapy to stop the disease is approved by the drug regulatory agencies, and the disease mechanisms remain poorly understood.
A new study carried out at the University of Eastern Finland analysed the causes behind loss of vision and detrimental retinal changes in CLN5 disease, i.e. the Finnish variant of NCL. The researchers used genetically modified mice in which the gene encoding the CLN5 protein had been made defective. In humans, malfunction of the gene leads to CLN5 disease.
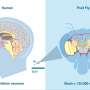
The researchers found that CLN5 deficient mice developed retinal degeneration long before reaching sexual maturity. Retinal function, especially associated with rod photoreceptors and the retinal pigmented epithelium cells, was reduced in young mice, and a similar phenomenon has been observed in several dog and sheep breeds with NCL. Scientific evidence on humans is inconclusive, but researchers believe that photoreceptor degeneration precedes the degeneration of other parts of the retina in humans as well.
Retinal protein analyses revealed that compared to age-matched controls, CLN5 deficient mice had abnormal levels of several autophagy related proteins in the retina. Earlier studies have observed similar changes and impaired lysosomal degradation in several distinct tissues from mice expressing other forms of NCL, including brain tissue. Lysosomal degradation is the final phase of autophagy, preventing the accumulation of detrimental waste materials in cells.
Normal visual function requires constant renewal of photoreceptors through lysosomal degradation. In CLN5 deficient mice, this degradation mechanism seems impaired, and this is why photoreceptors may die as the disease progresses, although detrimental pigment accumulation typical of NCL diseases can be observed in the entire retina. Similar retinal changes have also been observed in mice, dogs and sheep with several other forms of NCL, suggesting that the findings could apply to several forms of NCL. According to the researchers, the role of impaired lysosomal degradation in NCL-associated detrimental changes in the brain remains unknown.
"Non-invasive retinal examinations could possibly be used as biomarkers of central nervous system diseases", says Henri Leinonen, Ph.D., the first author of the article. In the future, retinal examinations may prove useful in studying treatment responses and disease progression in neurological diseases. Compared to brain examinations, retinal examinations have the advantage of being relatively cost-effective and safe. In NCL diseases, retinal examinations are used to study disease mechanisms in animals, and nowadays retinal examinations can also be used to support diagnosis in humans.
More information: Henri Leinonen et al, Retinal Degeneration In A Mouse Model Of CLN5 Disease Is Associated With Compromised Autophagy, Scientific Reports (2017). DOI: 10.1038/s41598-017-01716-1