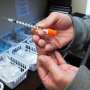
Campaigner with drug past warns of 'chemsex' HIV link
The sexual health expert credited with coining the term "chemsex" told AFP that drug-laced sexual encounters are boosting HIV infections in gay communities.
David Stuart, who manages the chemsex support programme at a pioneering clinic in Soho, was himself involved in drugs and escorting and contracted HIV before turning his life around after a 2005 arrest.
"These drugs are contributing phenomenally to the HIV epidemic," Stuart said in an interview at the clinic in the heart of London's gay community.
"They are not the drugs of the past—happy dancy drugs—they are much more problematic," he said.
Stuart defines chemsex as the "use of drugs for sex" which is "associated with certain behaviours such as hooking up online, high number of partners and high prevalence of HIV and sexually-transmitted disease."
Chemsex drugs, such as crystal methamphetamine, mephedrone and GBL "tapped into something that disinhibits sexual feelings," he said.
Condomless sex and communal drug use at chemsex parties are partly to blame for continued high levels of new HIV infections which have been at around 6,000 people a year since 2009.
"We have about 30 people coming to our building every day, perhaps because they have been exposed to HIV, maybe through condomless sex or sharing needles.
"We know that between 60 and 80 percent of those guys... are here because they have been in some kind of chemsex environment," he said.
Drugs 'part of our culture'
The practice mushroomed with the smartphone revolution, which has facilitated the buying of drugs and the hooking up of willing partners through smartphone apps such as Grindr.
But he believes focussing on the public health issues is to diminish the full impact that the trend is having on the community.
"GBL is a very dangerous drug," he said.
"One millilitre might be enough to give me the appropriate high I am looking for, 1.8 could kill me. One gay man dies every 12 days from GBL in London."
He added: "There are so many other harms associated to it: lifestyle and well-being, the ability to have sober sex, the ability to form intimacies and maintain them, getting to work on Monday, spending time with family and friends."
Sexual assault is also "very much something that is happening within our communities," he warned.
This was highlighted most tragically last year by the case of serial killer Stephen Port, who killed four men during chemsex sessions.
Stuart believes chemsex is an issue unique to the gay community due to its history of hedonism and of being defined by sexuality.
"Drugs are part of our culture, be that a good thing or a bad thing," he explained.
"When we were fighting for gay rights and fighting through the AIDS epidemic and when it was illegal to be gay, we came together on dancefloors, on drugs, as part of a community."
'Phenomenal' drop in HIV rates
Stuart moved to London from his native Australia in 1989—the same year he was diagnosed HIV positive.
He said he then spent years "either ill with AIDS, or recovering from one drug bender or another".
"Escorting and drug dealing were par for the course," he said.
He was arrested in 2005 and began to volunteer for an LGBT service within a drug charity.
Stuart started researching the links between HIV and chemsex, realising that sexual health services and gay charities were "much better suited" to deal with the issue than traditional drug services.
"With a lot of the guys, chems are being used to facilitate intimacy. Drugs are just taking away all that judgement and self-hatred," he said.
The treatment is complex, combining clinical solutions such as immediate treatment for new cases and the use of post-exposure prevention drugs along with education about using apps such as Grindr.
There is room for optimism, however.
Stuart said his clinic had seen a 42-percent fall in new HIV infections in the last six months.
"That's the first time in decades we've had such a phenomenal reduction," he said.
Synthetic seventh heaven: the perils of chemsex
"When you come down, you think: 'Oh God, how many people have I had sex with this weekend?'", says 30-something Briton James Wharton, recalling the anxiety that gripped him after a chemsex binge.
Wharton is not alone.
The practice of turbocharging sexual encounters with powerful drugs that peel back inhibitions and boost endurance has gripped parts of Europe's gay community, raising red flags among doctors and campaigners.
The dangers of "chemical sex" are many, including addiction, overdose and HIV infection, and the tally of victims appears to be mounting, they say.
"The increase of this phenomenon is visible in health services, whether for infectious diseases or addiction," said Maitena Milhet, a sociologist at the French Observatory for Drugs and Addiction and lead author of a study on chemsex published on Thursday.
Mixing sex and drugs—in couples, or in groups—is nothing new.
But the easy availability of evermore powerful synthetic molecules on the internet is: next-generation methamphetamines; the party drugs GBL—also known as 'coma in a bottle'—and GHB, which acts on the central nervous system; the stimulant cathinone found in khat leaves, traditionally chewed in east Africa.
Use of the drug cuts across gender and sexual orientation, but it is particularly a problem in part of gay culture, where it goes hand-in-hand with quick-sex dating apps such as Grindr and Scruff.
"With smart phones, you can do everything from the comfort of your sofa: order up the drugs and find sexual partners to share them with," said Fred Bladou, who helped set up an emergency chemsex hotline at the French association AIDES.
London, the epicentre
There are no official statistics, but activists and social workers across Europe all agree: chemsex remains a marginal phenomenon within the larger male gay community but is on an upward trend.
"London is probably known as the chemsex capital," said David Stuart, manager of the ChemSex support programmes at 56 Dean Street, a sexual health centre in the district of Soho.
Of the 7,000 to 8,000 gay men who come through the clinic's doors each month "3,000 are using chems and are coming here with the consequences of chemsex," he told AFP.
The risk of addiction is high, especially for gay men over 40, said Andreas von Hillner, a worker at gay counselling service Schwulenberatung Berlin.
"Many had rarely, or never, used drugs before, and very quickly, massively began consuming these hard drugs," he told AFP. "The addictive potential is very high."
Injecting the drugs—a practice known as "slamming"—is especially hazardous.
"These drugs are killing us," said Stuart.
Three of 21 overdose deaths in Paris in 2015 were attributed to slamming with cathinones. All three victims identified as part of the gay party scene.
Another dangerous side-effect is the tendency to withdraw socially into a drug-and-sex infused bubble.
"Chemsex is great when you're as high as a kite and you've got six or seven guys naked trying to pull you to one side of the room," said Wharton. "The gratification and validation of your body—it's incredible."
"But the downside... can have dramatic knock-on effects on other important parts of your life."
Craving intimacy
For two full years Wharton spent all his weekends in random apartments having drug-fuelled sex.
The former soldier and LGBT activist has written a book about his experiences to be published next week.
He was driven, he recalled, by a desperate search for intimacy. "You meet someone, sleep with them within an hour, and tell him very personal things. You get very close very quickly."
And then one day, he asked himself: "When is the last time I went to the cinema and saw a film, something I used to do quite often?"
That, Wharton said, is when he began to understand the emptiness and self-destructiveness of his lifestyle.
Arguably the greatest risk for "chemsexers" is how often they expose themselves—and others—to sexually transmitted disease.
"A lot of people stop using condoms when their sense of risk disappears" under the influence of the drugs, explained Ivan Zaro, a social worker in Madrid.
Scientists in Britain and Ireland have pointed to a surge in cases of gonorrhea and syphilis, including repeat infections, among chemsex users.
British researchers, in a survey of 30 HIV clinics in England and Wales, found that 29 percent of gay men who had the AIDS virus had been engaging in chemsex.
Sharing needles to inject chemicals also multiplies the risk of infection, especially among men with little experience of shooting up.
"When we enroll a chemsexer to the addiction centre, he finds himself in the midst of cocaine and heroin addicts and feels out of place," Zaro told AFP.
That is largely because, said Carsten Gehrig from the German NGO AIDS-Hilfe Frankfurt, "people who take drugs to enhance sex do not see themselves as addicts."
The German government has tasked a nationwide NGO, Deutsche Aids-Hilfe, with training health professionals in treating gay practitioners of chemsex, part of a project called Simdis.
Health campaigners say the best way of treating chemsex addiction is to reject hype and moralising—hard-won lessons from the 36-year war against AIDS.
"We should avoid alarmism, which is counterproductive," said Bladou. "The more we stigmatise people, the more we push them away from treatment."
© 2017 AFP