Faster diagnosis of inherited and lethal nerve disease could advance search for new treatments
Johns Hopkins physicians report success in a small study of a modified skin biopsy that hastens the earlier diagnosis of an inherited and progressively fatal nerve disease and seems to offer a clearer view of the disorder's severity and progression. With a quicker and less invasive way to visualize the hallmark protein clumps of the rare but lethal disease—familial transthyretin amyloidosis—the researchers say they hope to more rapidly advance clinical trials of treatments that may slow the disease and extend patients' lives.
In a report on their study, published June 20 as an Early View article online in Annals of Neurology, the Johns Hopkins team found that increasing levels of the protein clumps corresponded with worsening nerve damage, indicating that the smaller skin biopsies they used appear to work well as a measure of disease severity.
People with the transthyretin amyloidosis have mutations in the DNA of the transthyretin gene, which causes abnormal buildup and deposits of a transport protein called transthyretin in nerve and heart cells. Patients typically experience progressive pain, muscle weakness and ultimately kidney, heart and other organ failure, with the disease usually manifesting itself in people ages 40 to 60. Although precise estimates of the disease's prevalence are unknown, the disorder is rare, striking about 1 in 100,000 Americans of European descent; the rates are thought to be higher in African Americans.
"In the last few months, we've diagnosed several people with the disease years before the diagnosis is typically made, which has changed how we do medicine in our nerve clinic," says Michael Polydefkis, M.D., professor of neurology at the Johns Hopkins University School of Medicine and senior author on the study.
Polydefkis, also director of the Cutaneous Nerve Lab at the Johns Hopkins Bayview Medical Center, says that patients with transthyretin amyloidosis typically have traditional symptoms of nerve damage, known as neuropathy, such as numbness or burning in the feet. But unlike typical neuropathy patients, transthyretin amyloidosis patients develop more rapid progression of their disease as well as additional symptoms, such as problems with their digestion and irregular heartbeat, within about three to five years.
Traditionally, a firm diagnosis of the disorder requires a surgical nerve biopsy followed by genetic tests. From initial onset of symptoms, patients on average live about 10 to 12 years.
Over the past few years, Polydefkis and his team have developed a skin biopsy he uses to diagnose other types of nonfatal neuropathies by measuring the number of nerve fibers in the skin samples taken from the leg. The skin biopsy takes a small, 3 mm-wide sample of tissue (about half the width of a pencil eraser) and can be performed in a doctor's office.
The new study was designed to see if a faster and better diagnosis could be made for transthyretin amyloidosis using a modified version of the skin biopsy technique.
For the study, his group recruited 30 patients with six different genetically-confirmed transthyretin amyloidosis mutations. Twenty patients had neuropathy symptoms and 10 did not. They also recruited 20 age and gender-matched healthy controls, and 20 age and gender-matched patients with diabetic neuropathy—a different form of peripheral nerve damage due to high blood sugar. Participants ranged in age from 17 to 83; 42 percent were women.
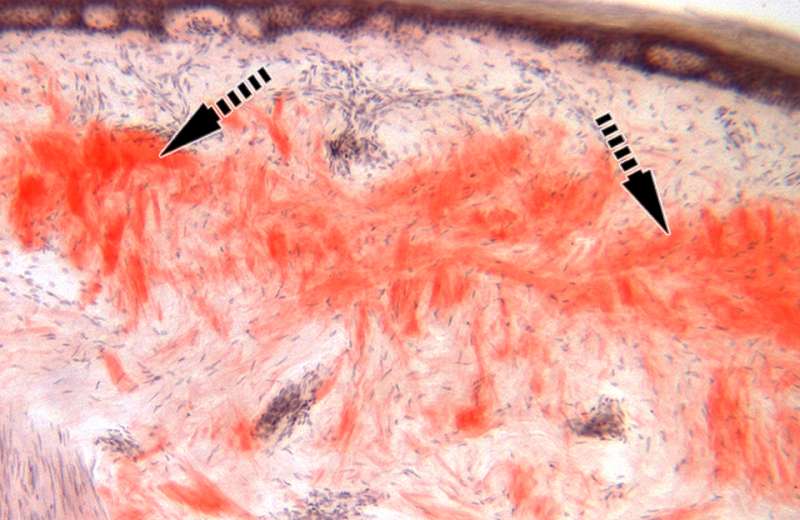
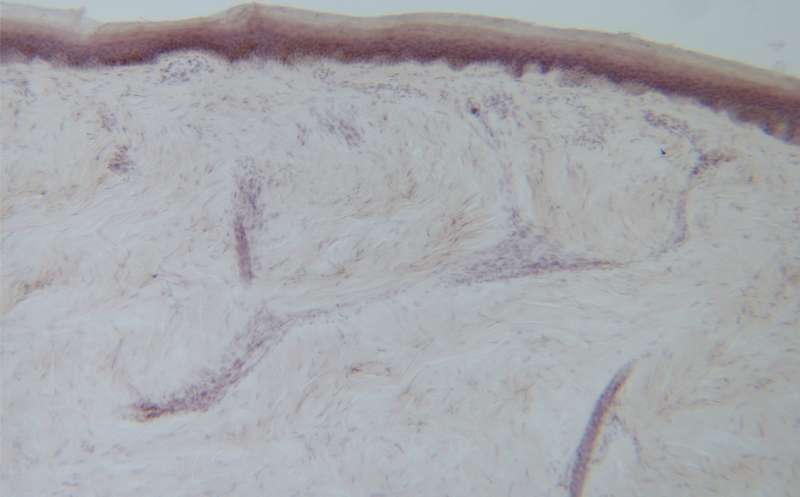
Each subject had skin biopsies taken from their outer ankle and upper thigh. The biopsies were thinly sliced and stained with a dye called Congo red that allowed the researchers to view the protein clumps in the layers of skin or within the sweat glands and pilomotor muscles (those that cause goose bumps) under the microscope. These red protein clumps looked yellowish-green when observed with a polarized lens distinguishing them from other structures in the skin sample.
Researchers observed the protein clumps in 14 people with symptoms of neuropathy and the disease and in two people with the disease but without accompanying neuropathy symptoms. The protein clumps weren't seen in any of the healthy controls or in samples from people with diabetic neuropathy.
Based on their results, Gigi Ebenezer, M.B.B.S., M.D., assistant professor of neurology and the first author on the study, reported that protein clumps were detected in 70 percent of cases and 20 percent of patients who carried disease-causing genes but hadn't yet developed symptoms. None of the control cases showed amyloid.
The researchers also examined skin slices from two patients with another form of nerve disease called AL amyloidosis, caused by a bone marrow disorder. They also could see red protein clumps in the skin samples of these people, sparing them a more invasive nerve biopsy.
Next, the researchers compared the quantity of protein clumps compared to the level of disability in the lower legs of each participant. The quantity of protein clumps was calculated using a computer program that measured the amount of tissue in a skin slice with protein clumps expressed as a percentage of the tissue's total area. The disability score ranged from 0 (no disability) to 88 (severely disabled) and incorporated measurements of sensation, muscle power, tendon reflexes and electrical activity in the leg nerves.
The average disability score in healthy participants was 0.2. In patients with transthyretin amyloidosis but no symptoms, the average score was 4.4 and in patients with the disease and neuropathy symptoms the average score was 31.8. Healthy controls had an average of 0 percent protein clumps in their skin samples, while those with transthyretin amyloidosis but no symptoms had an average of 0.4 percent protein clumps and symptomatic patients with the disease had an average of 26.3 percent protein clumps. Higher percentages of protein clumping corresponded to greater disability in people with transthyretin amyloidosis.
"The disability level aligned with the quantity of amyloid (protein clumps) present makes intuitive sense, but we were really amazed that the information from a small skin biopsy would correlate so well with disease severity," says Polydefkis. "It suggests that what we find in the skin reflects what the disease is doing in the rest of the body."
He cautions that his group only tested the six most common transthyretin mutations and that hundreds of other mutations exist in the gene that may not show similar patterns.
"But if further studies confirm and extend what we have found, we may use the skin biopsy as a biomarker for disease severity. And we will be able to diagnose more patients sooner, which is important for patients and their families so they can begin planning for the future," says Polydefkis. "The good news is that drug companies are using our skin biopsy technique in ongoing clinical trials to monitor treatment success." He says results from phase II and III trials on these new therapies designed to stall the disease are slated to come out within the year.
The incidence of transthyretin amyloidosis worldwide is unknown, according to the U.S. National Library of Medicine. People of African descent may have rates as high as 3-5 percent.
More information: Gigi J. Ebenezer et al. Cutaneous nerve biomarkers in transthyretin familial amyloid polyneuropathy, Annals of Neurology (2017). DOI: 10.1002/ana.24972













