Some developed countries should target adolescents and adults for measles vaccination
Even if measles infection incidence has decreased by at least 90 percent all over the world since the introduction of the vaccine, measles is still one of the major causes of death in children among vaccine-preventable diseases. Regular measles epidemics are reported in developing countries and recurrent episodic outbreaks occur in the developed world.
A new study by Bocconi University and Bruno Kessler Foundation analyzing nine countries (Australia, Ethiopia, Kenya, Ireland, Italy, South Korea, Singapore, the UK, the US) and published in The Lancet Infectious Diseases, highlights the role played by demographics in the spread of measles and concludes that future vaccination strategies in high-fertility countries should focus on increasing childhood immunization rates, while immunization campaigns targeting adolescents and young adults are required in low fertility countries.
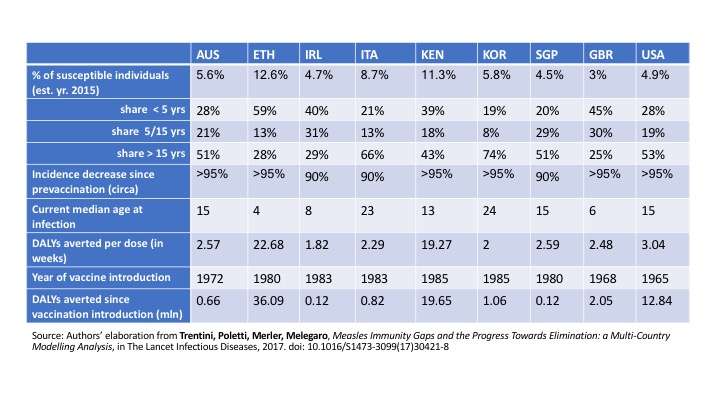
Using a transmission model calibrated on historical serological data the authors estimate that the susceptible proportion of the population (i.e. unprotected against the infection) varies from ca. 3 percent in the UK to more that 12,5 percent in Ethiopia, with astonishing differences in its age-composition, due to different vaccination strategies and divergent demographic trends. While the percentage of over-15 among susceptible individuals in Ethiopia and Kenya is, respectively, 28 percent and 43 percent, adolescents and young adults represent 74 percent of unprotected individuals in South Korea, 66 percent in Italy and 53 percent in the US, with considerable immunity gaps in individuals aged 30-40 years.
"Every effort to increase the vaccination coverage rate among children is praiseworthy", says Alessia Melegaro, a Bocconi professor and principal investigator of DECIDE, the ERC-funded project which produced the article, "but in some developed countries it's the lack of coverage among adolescents and adults that poses a serious threat to the goal of eliminating measles.".
"Measles incidence could increase, in the next decades, in Italy, Australia and Singapore and Ethiopia is at high risk of future large epidemics", says Stefano Merler from Bruno Kessler Foundation, "and this is particularly worrying considering that individuals get infected later in life when the disease is more severe. The median age at infection for 2015 was estimated to be 5–10 years in the UK, Ireland, and Ethiopia; 10–15 years in the USA, Australia, Singapore, and Kenya; and older than 20 years in Italy and South Korea".
The proposed model shows that the introduction of the measles vaccine, which occurred at different times in the nine countries, has considerably reduced the disease burden in terms of disability-adjusted life-years (DALYs), a measure expressed as the number of years lost because of illness, disability, or early death. Every vaccine dose averts two or three weeks of DALYs in the developed world and around 20 weeks in Kenya and Ethiopia. Which translates into 2-mln years since the vaccine introduction in the UK, 13-mln in the US and 36-mln in Ethiopia.
"Vaccination has undoubtedly achieved incredible results in terms of public health. In particular," continues Prof. Melegaro "our analysis showed that routine first dose vaccine administration has been responsible for more than 90 percent of the overall number of vaccine-immunized individuals in most countries. In Ethiopia and Kenya, catch-up and follow-up campaigns substantially mitigated the effect of suboptimum routine vaccine coverage, generating 25-45 percent of the immunized fraction of the population. Tailoring immunization campaigns to achieve measles eradication goals is essential and currently, for some countries, this means considering also the role of unprotected adolescents and young adults".
More information: Filippo Trentini et al. Measles immunity gaps and the progress towards elimination: a multi-country modelling analysis, The Lancet Infectious Diseases (2017). DOI: 10.1016/S1473-3099(17)30421-8
















