Prostate cancer testing: has the bubble burst?
In 2010, I wrote a free book on prostate cancer testing with two colleagues, Alex Barratt (an epidemiologist) and Martin Stockler (a clinical oncologist), Let sleeping dogs lie? What men should know before getting tested for prostate cancer. It has been downloaded just short of 38,000 times, the highest of any item in Sydney University's open access repository.
Clearly, there is understandably immense concern about prostate cancer. In 2014, 3,102 Australian men died from the disease, making it the second leading cause of cancer death in males after lung cancer (4,947 deaths).
Media reporting about prostate cancer testing has long emphasised screening as highly sensible. This is consistent with other early-detection cancer-control messages about "finding it early".
However, news reports often neglect to mention or minimise adverse consequences of interventions following the surgery and radiation that can follow a positive screening test, like long-term sexual impotence and incontinence.
There's also a pitch to gender equity ("women have their cancer tests, and men have this one"). Those questioning testing have been vilified, and epidemiological details framed as an inferior form of knowledge than clinical experience.
Ten years ago, a study of Australian media reports found 10% of a large sample of statements in news reports were inaccurate or misleading and concluded:
Despite near universal lack of support for prostate cancer screening of asymptomatic men by leading international and Australian cancer control agencies, Australians are exposed to an unbalanced stream of encouragement to seek testing. This coverage includes inaccurate information which ignores scientific evidence and the general lack of expert agency support.
Since we published our book, many men have contacted me thanking us for writing it. But I've also been taken aside by others with this message: "Look, I know about all the controversy about prostate cancer testing but my husband had the test and his doctor said he was so lucky that they found it early because it was very advanced and if they'd left it any longer, he'd have almost certainly died from it."
I reply that I of course have no idea what the test and subsequent biopsy showed and so I could not possibly comment. In some cases, this will be true, but as we shall see, in many more cases it won't be.
Why are men unlikely to question advice?
People who have been told by a specialist urologist that they are at serious risk of death are naturally unlikely to question what they are told. Having climbed on board the testing, biopsy and radical treatment "train" and being still alive to tell their story, they have what is often called "survivor joie de vivre".
They are utterly convinced that the cancer discovery and radical intervention (surgical prostate removal or radiation therapy) has saved their lives. They can be evangelical about their luck, even when 77% live with sexual impotence three years after surgery. As some will tell you, "you can't have sex in a coffin".
But such accounts do not tell us whether testing and subsequent intervention really save lives. Here, the evidence needs to come from longitudinal studies of men who found to have elevated prostate specific antigen (PSA) test results (including men who have not been tested) and who are then randomised into different treatments (including no treatment).
Seven years after we summarised available knowledge on this in our 2010 book, we now have results from two recent clinical trials to help us make even stronger informed decisions: the Prostate Testing for Cancer and Treatment (ProtecT) – 10 years of follow-up - and Prostate Cancer Intervention versus Observation Trial (PIVOT) – 20 years of follow-up.
Two Australian oncologists, Ian Haines and George Miklos, have given us an important, excoriating summary of these two studies. They conclude the data:
… completely undermine the stratospheric spin associated with prostate cancer being a death sentence. They are unambiguous in their implications … The bottom line? Men with early stage abnormalities of the prostate who do not undergo surgery or radiation treatment, but whose condition is monitored for any progression of the cancer, live just as long as men who opted for complete removal of the prostate and who now live with its immediate consequences, including incontinence, intimacy issues, bowel problems and intervention regret.
What do the data say?
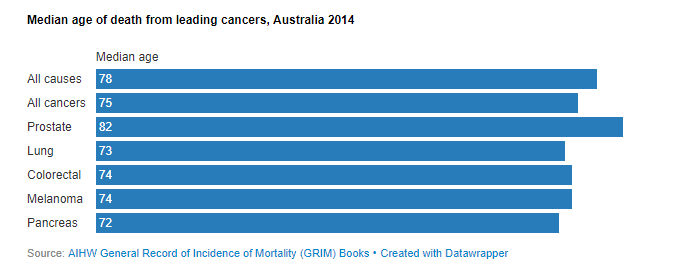
The Australian Institute of Health and Welfare (AIHW) collates all incidence and mortality data for all cancers. This table shows the average age of death in men from various cancers and all causes of death combined for 2014, the latest available year.
This shows that prostate cancer is very clearly a disease that mostly kills very late in life. The average age of death for prostate cancer in Australia is 82 years, while the average age for all male cancers combined (other than prostate cancer) is 75 – considerably younger.
Sixty percent of men who die from the disease are aged 80 or over with 87% aged 70 or more. Just 2.1% (65 men) who died from the disease were aged under 60, and three (0.1%) were aged under 50.
Significantly, the average age of death (from all causes combined) for an Australian man in 2014 was 78 years.
So men who die from any cause after that time – prostate cancer included – are already living longer than average. Prostate cancer is one disease in the Grim Reaper's quiver at the end of our lives. As we all must will die from some cause, it's worth reflecting on why so much attention should be given to a disease that stands out so obviously as one that kills most very late in life.
In 2014, prostate cancer killed 3,102 males out of 78,341 deaths from all causes (4%). It's long been remarked that far more men die with prostate cancer than from it. We know from autopsy studies that around 40% of men in their 40s will have signs of prostate cancer, with this increasing to about 60% of men in their 60s. Clearly then, the great majority of men who develop prostate cancer will not die from it but from something else.
Yet the drive to promote prostate testing continues unabated, which is causing massive anxiety, intervention and significant decrements to the quality of life of men who are treated unnecessarily. Haines and Miklos point the finger at financial reasons for this over-treatment.
It will be even more difficult to dislodge early PSA testing, particularly in countries such as the United States, where it has now become deeply entrenched in a belief-based or business enterprise. After all, given the huge investments in proton-based radiation facilities (where it costs in excess of $300 million to just build a proton beam facility), or in robotic surgery machines, the financial incentives to repay the investment and to move to a for-profit situation are huge. A constant supply of patients is obligatory, and an increasing supply is preferable.
Many male doctors do not have PSA tests themselves. As more information emerges that challenges the wisdom of the promotion of prostate testing, we need to ask whether this bubble is near to bursting.
This article was originally published on The Conversation. Read the original article.![]()