Why these sperm are the key to the future of fertility – and contraception

Despite the huge global demand for both fertility treatment and contraception, there are surprisingly few options to boost male fertility, or for male contraception. To have more options, we really need a better understanding of how human sperm work. Unfortunately, they are incredibly difficult to study in the lab.
Not only are sperm the smallest cells in the body (25 times smaller than a grain of sand), they are unique and highly specialised, designed to survive outside the body. Unlike other cells, sperm contain virtually no cytoplasm – the jelly-like fluid that fills a cell and stores many of the chemicals that are essential for life. Instead they interact with the surrounding environment to inform their behaviour. Their internal chemical messages and signals are also different to those of other cells, meaning we can't make assumptions about how they work and many standard cell research techniques can't be applied in the lab. It's little wonder then that research in the field of male fertility and contraception is limited.
Growing infertility
Infertility is estimated to affect about one in six couples of reproductive age (in France). Male fertility problems are increasingly common. However, our limited understanding of how sperm work and the requirements needed to achieve fertilisation, means that we struggle to treat this problem.
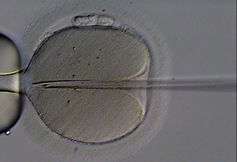
Incredibly, there is no drug that an infertile man can take, or that can be added to his sperm in a laboratory to improve how sperm swim or work. Instead couples rely on treatments such as in vitro fertilisation (IVF) and intracytoplasmic sperm injection (ICSI), which are expensive, invasive, and not guaranteed to succeed. Nonetheless, the number of people seeking IVF and ICSI treatment is increasing each year.
Contraception
Although access to female contraception varies considerably across the globe, use of male methods (condoms, vasectomy) is consistently low. There has been no significant innovation in available male contraception in the past 50 years. Hormonal and non-hormonal methods have been researched since the 70s, but side effects were too severe for implementation.
New, safe, effective and acceptable contraceptive methods for men would help to address the needs of couples who do not, or cannot, use currently available methods. Having a wider choice of contraceptives is also known to increase uptake of all methods. Perhaps more significant is the potential to give men increased options in family planning, levelling the gender inequality in this area.
Silent swimmers
There is a real demand – and an unmet need – for the development of new treatments for both male infertility and family planning. But, before we can tackle these global health issues, we need to understand how sperm work. Without this detailed knowledge, and a potential target for a drug to work on, it is virtually impossible to develop new compounds to enhance, or inhibit, sperm function.

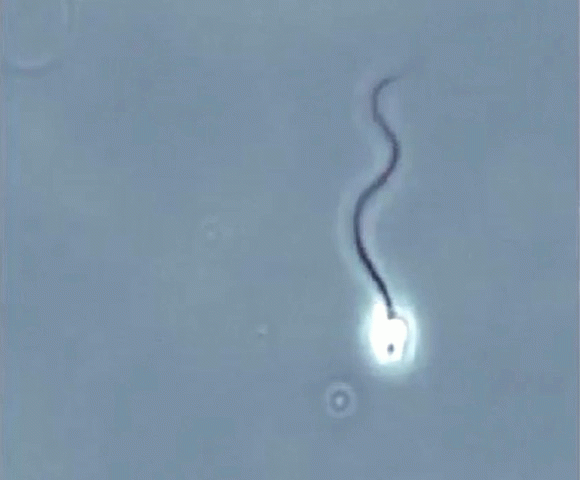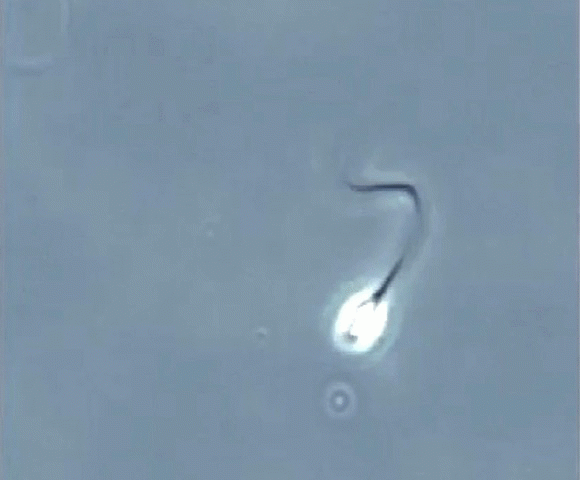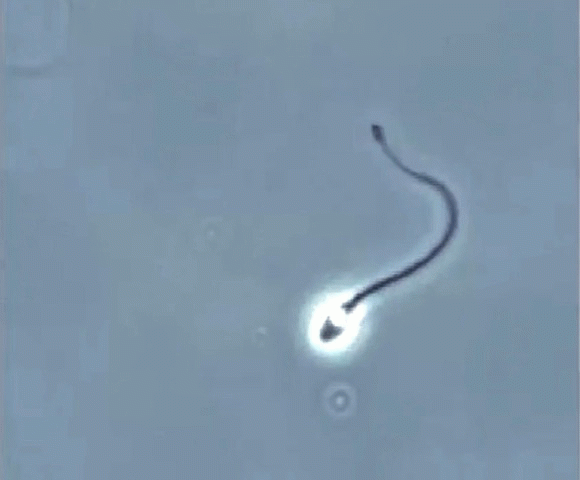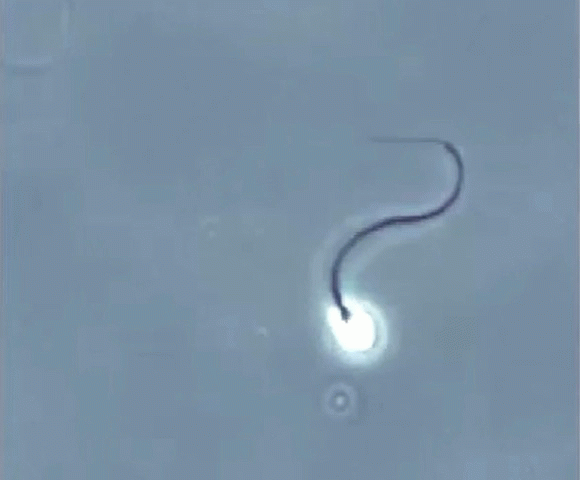
Sperm swimming (motility) is probably its most important characteristic. Although the underlying cellular mechanisms are not fully understood, changes in levels of calcium inside the sperm cell are known to be crucial to sperm function, including swimming and fertilisation. Fluctuations in the level of calcium within sperm cells is known to be due to specific membrane pores (ion channels) in the sperm tail – these pores are called CatSper.
High-throughput screening (HTS) is an approach used by the pharmacology industry to discover new drugs, where automated experiments can examine thousands of compounds to "screen" for a desired effect. Compounds that show the desired effect are called "hits".
We recently published a paper describing a HTS approach to look for new drugs to treat male infertility. Calcium inside sperm was fluorescently labelled, and levels then measured in response to a number of new drug compounds.
We screened more than 3,400 compounds and identified 48 hits, that showed the effects we needed. Further testing of several of these hit compounds found two that showed improved function and swimming in sperm, probably due to an effect on CatSper channels.
A potential cure
Although the original experiments used sperm from healthy volunteers, the researchers also saw enhanced function and swimming when they tested both compounds on samples from patients undergoing IVF. Given the lack of progress in treating male infertility to date, this is a promising find, even if it is very early days.
The beauty of this finding is that the compounds that we found would only act on sperm cells, because the ion channel "CatSper" is unique to sperm. This could help to avoid unwanted side effects, which makes these compounds attractive clinically and commercially. While this research has been directed at drug discovery for male fertility, it is possible to turn the concept around and find compounds that inhibit sperm swimming, thereby creating a new male contraceptive.
This is an advance that potentially offers hope to millions of couples worldwide, but there is still much that we need to know and understand to unlock the workings of the human sperm.
This article was originally published on The Conversation. Read the original article.![]()


















