September 11, 2017 report
Bisphenol A exposure through the skin from store receipts takes longer to be excreted
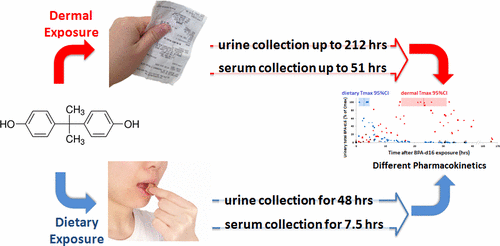
(Medical Xpress)—A pair of researchers, one with the University of Alberta the other with Stockholm University, has found that it takes longer for people to excrete bisphenol A from the body than when the compound is consumed. In their paper published in the journal Environmental Science & Technology, Jiaying Liu and Jonathan Martin describe their research and why they believe their findings suggest a trip to the store could present a health hazard for consumers.
By now, most everyone has heard of bisphenol A (BPA), a synthetic compound often used when making plastics and epoxy resins. It has been in the news over the past couple of years as reporters learned that it was used in baby bottles and other containers. Many industries have since banned such applications, but the risk remains due to its continued use in other products. In this new effort, the researchers report that not only is BPA introduced into the body when handling register receipts from stores, but lasts longer in the body when introduced through the skin.
BPA, the researchers note, is often used in the manufacture of thermal paper—the type used in many store registers. It is what causes the color change we see as sales data. But they also note that in handling such receipts, consumers inadvertently expose themselves to BPA as it seeps in through the skin.
To learn more about the possible impact of BPA absorption through such receipts, the researchers asked volunteers to eat cookies with a few micrograms of the compound and then monitored BPA in their urine as it was excreted. The researchers report that all traces of BPA in the urine were gone from all the volunteers within 24 hours of ingestion. In the second part of the study, the researchers had the volunteers handle register receipts and then monitored their urine as well. In this case, the researchers report, levels of BPA continued to rise in the urine for approximately two days. Also, strikingly, half of the volunteers still had traceable amounts of the compound in their urine after a week.
The researchers conclude that BPA absorbed through the skin takes longer to excrete and therefore those who handle store receipts endure more toxic exposure.
More information: Jiaying Liu et al. Prolonged Exposure to Bisphenol A from Single Dermal Contact Events, Environmental Science & Technology (2017). DOI: 10.1021/acs.est.7b03093
Abstract
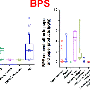
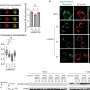
Bisphenol A (BPA) is an endocrine disruptor frequently detected in human biofluids. Dermal absorption of BPA from thermal paper receipts occurs but BPA pharmacokinetics following dermal exposure is not understood. To compare the pharmacokinetics of dermal and dietary BPA exposure, six male participants handled simulated receipts containing relevant levels of BPA (isotope-labeled BPA-d16) for 5 min, followed by hand-washing 2 h later. Urine (0–48 h) and serum (0–7.5 h) were monitored for free and total BPA-d16. One week later, participants returned for a dietary administration with monitoring as above. One participant repeated the dermal administration with extended monitoring of urine (9 days) and serum (2 days). After dietary exposure, urine total BPA-d16 peaked within 5 h and quickly cleared within 24 h. After dermal exposure, cumulative excretion increased linearly for 2 days, and half the participants still had detectable urinary total BPA-d16 after 1 week. The participant repeating the dermal exposure had detectable BPA-d16 in urine for 9 days, showed linear cumulative excretion over 5 days, and had detectable free BPA-d16 in serum. Proportions of free BPA-d16 in urine following dermal exposure (0.71%–8.3% of total BPA-d16) were generally higher than following the dietary exposure (0.29%–1.4%). Compared to dietary BPA exposure, dermal absorption of BPA leads to prolonged exposure and may lead to higher proportions of unconjugated BPA in systemic circulation.
© 2017 Medical Xpress