Revisiting abandoned treatments in fight against antimicrobial-resistant gonorrhea
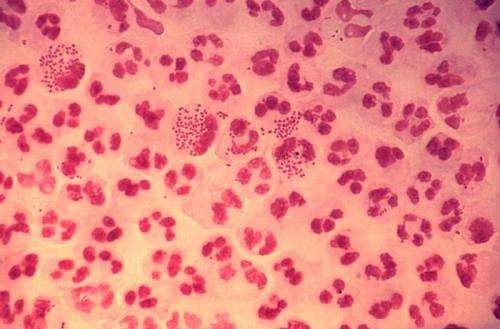
A previously recommended treatment for gonorrhea, cefixime, may be an effective alternative to current treatments as clinicians battle outbreaks and emergence of antimicrobial resistance (AMR), according to a study published this week by Xavier Didelot of Imperial College London, UK, and colleagues in PLOS Medicine.
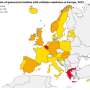
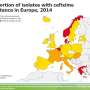
Gonorrhea, caused by the bacteria N. gonorrhoeae, is one of the most common sexually transmitted infections in England, and incidence has increased in recent years, particularly among men who have sex with men (MSM). Treating gonorrhea is complicated by the rapid development of antimicrobial resistance (AMR). The cephalosporin antibiotic cefixime was a recommended first-line treatment for gonorrhea before increasing prevalence of cefixime-resistant strains of N. gonorrhoeae was observed around 2010, leading to the removal of cefixime from treatment guidelines. While the currently recommended dual therapy of ceftriaxone-azithromycin remains effective, emerging ceftriaxone resistance has led to fears thaat this regimen may in turn become inadequate.
To determine whether re-introduction of cefixime treatment in a minority of cases might provide an effective alternative and help prevent emergence of resistance to ceftriaxone-azithromycin, the researchers developed a mathematical model of the dynamics of cefixime resistance observed between 2008 and 2015. The model includes a fitness benefit of cefixime resistance in N. gonorrhoeae during periods of wide use of the antibiotic (explaining the increase in resistant strains up to 2010) and a fitness cost of resistance (explaining the decrease in cefixime resistance after 2010). The model estimates treating cefixime-resistant gonorrhea with cefixime to be unsuccessful in 83% (95% credible interval [CrI] 53%-99%) of cases, representing a fitness benefit of resistance large enough to counterbalance the fitness cost to N. gonorrhoeae when more than 31% (95% CrI 26%-36%) of cases are treated with cefixime. The authors therefore suggest that cefixime could be used to treat up to 25% of gonorrhea cases without risk of cefixime resistance re-emerging.
The authors note that epidemiological data for their model is restricted to MSM, the population in which the cefixime-resistant outbreak of gonorrhea was concentrated, and that assumptions made to keep the model simple and generalizable may impact predictions.
In an accompanying Perspective, Magnus Unemo of Orebro University Hospital, Orebro, Sweden, and Christian Althaus of the University of Bern, Switzerland, discuss the value of modelling studies to inform AMR management. They also note the limitations of the current evidence base informing such models, highlight the need for studies measuring the many factors that affect transmissibility of resistant strains, and suggest caution before widely reintroducing antimicrobials such as cefixime.
Both papers are included in the new PLOS Medicine Collection on Sexually Transmitted Infections.
More information: Whittles LK, White PJ, Didelot X (2017) Estimating the fitness cost and benefit of cefixime resistance in Neisseria gonorrhoeae to inform prescription policy: A modelling study. PLoS Med 14(10): e1002416. doi.org/10.1371/journal.pmed.1002416