Newly published research provides new insight into how diabetes leads to retinopathy
An international team of scientists led by Professor Ingrid Fleming of Goethe University, Frankfurt, Germany, and including Professor Bruce Hammock of the University of California, Davis, provides new insight into the mechanism by which diabetes leads to retinopathy and often to blindness.
An inhibitor to the enzyme, soluble epoxide hydrolase (sEH), discovered in the Hammock lab, prevented the eye disease in diabetic mice, Fleming said.
The paper, "Inhibition of Soluble Epoxide Hydrolase Prevents Diabetic Retinopathy," involving six years of research and 22 scientists, is published today (Dec. 6) in the journal Nature.
"This has been a long but exciting project where Dr. Fleming's team used tools developed to study the biology of fatty acid epoxides to probe the fundamental mechanism of diabetic retinopathy," said co-author Hammock, a distinguished professor of entomology who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center "This work has targeted many possible sites for intervention that could preserve vision, and one such target is using inhibitors of the soluble epoxide hydrolase which block diabetic retinopathy in mice."
Fleming, who directs Goethe University's Institute for Vascular Signaling, Centre for Molecular Medicine, said a major cause of blindness stems from diabetes "where there is a loss of vascular cells in the retina of the eye, loss of barrier function in vessels, edema, and a cascade of inflammatory events leading to blindness."
The eye generates a dihydroxy metabolite from polyunsaturated fatty acids that initiates pericyte loss and breakdown of the endothelial barrier function in the eye, the scientists said. This leads to vascular edema and ultimately to a proliferation of new blood vessels and loss of vision.
The small molecule which initiates this process is a diol of a long chain poly unsaturated fatty acid produced by sEH, the researchers said. The enzyme converts an anti-inflammatory epoxy fatty acid into the pro inflammatory and in this case, toxic diol. The research team demonstrated this process and the cellular mechanism involved in diabetic mice and in transgenic mice that over-produce the sEH enzyme.
They were able to block the process by inhibiting the sEH enzyme. The expression of the sEH enzyme also increased with severity of diabetic retinopathy in human patients.
"The expression of the soluble epoxide hydrolase gene was shown to increase in the retinas of human patients with the severity of the disease with non-proliferative diabetic retinopathy," Hammock said. "Thus, there appears a connection to human medicine."
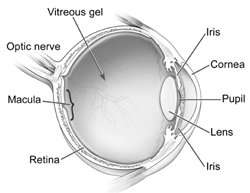
Diabetic retinopathy is the most common diabetic eye disease and a leading cause of adult blindness. Chronically high blood sugar from diabetes damages the tiny blood vessels in the retina, leading to diabetic retinopathy, according to the National Eye Institute (NEI) of the National Institutes of Health. The blood vessels can leak fluid or hemorrhage, distorting vision. NEI officials predict that the number of Americans with diabetic retinopathy will nearly double from 7.7 million in 2010 to 14.5 million by 2050.
Fleming said the sEH enzyme generates a toxic metabolite, but when the enzyme is inhibited, eye disease is prevented.
Earlier work reported in the Proceedings of the National Academy of Sciences from the Kip Connor laboratory at Harvard University showed that inhibiting the soluble epoxide hydrolase preserves fatty acid epoxides which reduce the late or proliferative stages of diabetic retinopathy and macular degeneration. Now the Fleming team used the same soluble epoxide hydrolase inhibitors to block production of a pro inflammatory mediator that initiates the early stages of vascular permeability and inflammation of the retina.
Connor, an assistant professor of ophthalmology at Harvard Medical School, praised the work as bringing to light "a previously unknown mechanism of action." Said Connor: "The identification by the laboratories of Drs. Fleming and Dr. Hammock that 19,20-dihydroxydocosapentaenoic acid, a product of soluble epoxide hydrolase (sEH) activity, as a key regulator of pericyte loss and endothelial barrier breakdown has brought to light a previously unknown mechanism of action in the induction of diabetic retinopathy. Moreover, the authors clearly show that inhibition of sEH blocks formation of this degenerative lipid metabolite thereby halting disease progression, which is of vital interest for the potential management of this blinding disease.
Mehran Moghaddam and David Grant, then with the Hammock lab, demonstrated that the diol of the fatty acid linoleate produced by the soluble epoxide hydrolase was highly toxic to cells leading to vascular permeability and sepsis. They published their work in 1997 in Nature Medicine.
"It is interesting how discoveries of years ago resurface as a critical lead in another disease indication," commented Moghaddam. "It certainly seems hopeful we will be able to treat blindness resulting from severe diabetes."
The Hammock laboratory has published almost 900 peer-reviewed papers on the sEH enzyme, discovered while Hammock and Sarjeet Gill (now of UC Riverside) were researching insect developmental biology and green insecticides at UC Berkeley. The work, begun in 1969, led to the discovery that many regulatory molecules are controlled as much by degradation as by biosynthesis, Hammock said. These epoxy fatty acid chemical mediators control blood pressure, fibrosis, immunity, tissue growth, pain and inflammation to name a few processes, and now Fleming's team has shown the diols products from these epoxides can cause diabetic retinopathy.
For many years Gill and Hammock were alone in studying this enzyme but today its importance is well recognized in mammalian biology, with more than 17,000 peer-reviewed papers in the area. Hammock credits the National Institute of Environmental Health Sciences (NIEHS) for supporting research in this area since the 1970s.
A Davis-based company, EicOsis, has received a large grant from the U.S. National Institutes of Health to move inhibitors to the clinic to treat diabetic neuropathic pain. "We are developing a non opiate analgesic to treat the chronic pain often associated with diabetes," said William Schmidt, vice president of clinical development at EicOsis. "It would be wonderful if the came drug also could be used to prevent the blindness driven by diabetes."
More information: Jiong Hu et al. Inhibition of soluble epoxide hydrolase prevents diabetic retinopathy, Nature (2017). DOI: 10.1038/nature25013
















