Heart cells sense stiffness by measuring contraction forces and resting tension simultaneously
Researchers from Queen Mary University of London have identified a new mechanism in which adhesive structures within the cells of the heart sense stiffness through muscle contractions and resting tension at the same time.
The study, published in Developmental Cell, further shows that the resting tension in the heart cells is increased after a heart attack and other heart diseases. This changes the way that heart cells can sense the stiffness because they lose sensitivity.
This suggests that abnormal mechanosensing and signalling, which occurs when the resting tension is increased, is a contributing factor in the progression of heart disease towards heart failure. When the cells misread the properties of their environment this will lead to heart cells that cannot beat as well.
Lead author Dr Thomas Iskratsch, from Queen Mary's School of Engineering and Materials Science, said: "This study develops our understanding of the disease mechanisms. It shows that changes to the heart after a heart attack contribute to the disease in two ways. On the one hand it changes the mechanical properties of the heart and on the other hand it changes how heart cells measure and respond to these properties."
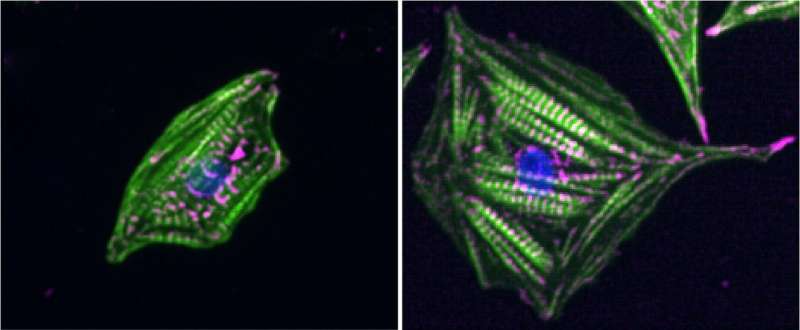
The stiffness of the cellular environment can guide cellular processes, from cell migration to differentiation or cell death. Many organs change the stiffness during development, ageing or disease. For example the heart becomes stiffer as it is formed in the embryo and it stiffens further in various heart conditions, mainly due to fibrosis.
Such changes in stiffness are known to impact the phenotype - or the look and behaviour - of the heart muscle cells and their ability to beat efficiently. However up until now it was unclear how the cells can measure the stiffness.
By identifying the mechanism in which adhesive structures within cells sense contractions and tension, the researchers found this combination of forces leads to the stretching of talin, a mechanosensitive protein on the intracellular side of the adhesions. Stretching of talin will then initiate a series of events that includes strengthening of the adhesions and signalling to the nucleus to change the cell phenotype.
Depending on the stiffness of the environment, this results in cyclic stretching of talin (when the stiffness is comparable to the healthy adult heart), continuous stretching of talin (when the stiffness is comparable to the diseased, fibrotic heart), or no stretching of talin (when the stiffness is comparable to the embryonic heart). The researchers also found indications for higher resting tension in heart disease, which again will shift the balance from cyclic to continuous stretching of talin.
Dr Iskratsch added: "Further steps are needed to investigate how the different types of talin stretching are translated into changing the cell behaviour. Also, more experiments are needed to observe the changes in mechanical sensing in the diseased heart. Together this will allow the identification of targets for new drugs."