Infant mortality rates in Texas vary dramatically from one zip code to the next: study
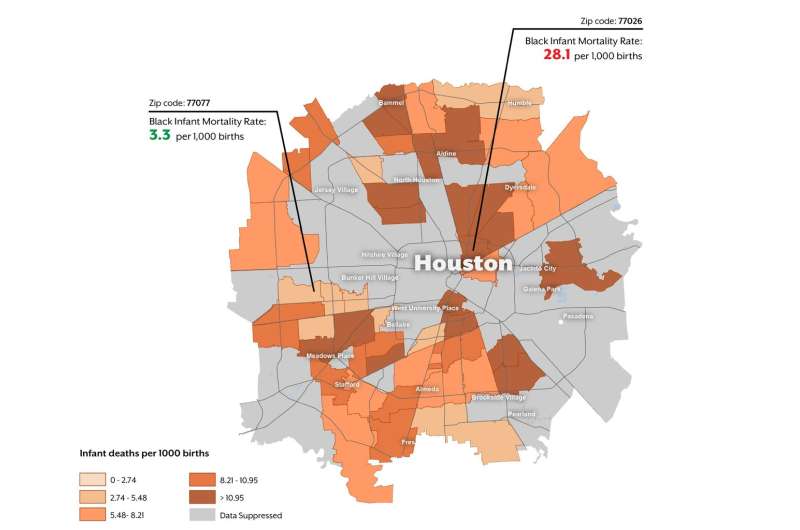
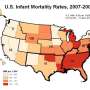
Infant mortality rates in Texas vary dramatically even across neighboring zip codes, according to a new analysis and mapping tool from researchers at The University of Texas System and UT Health Northeast. The analysis and searchable map, which are the first of their kind in Texas, use data from Texas Vital Statistics Linked Birth and Death Records from 2011-2014.
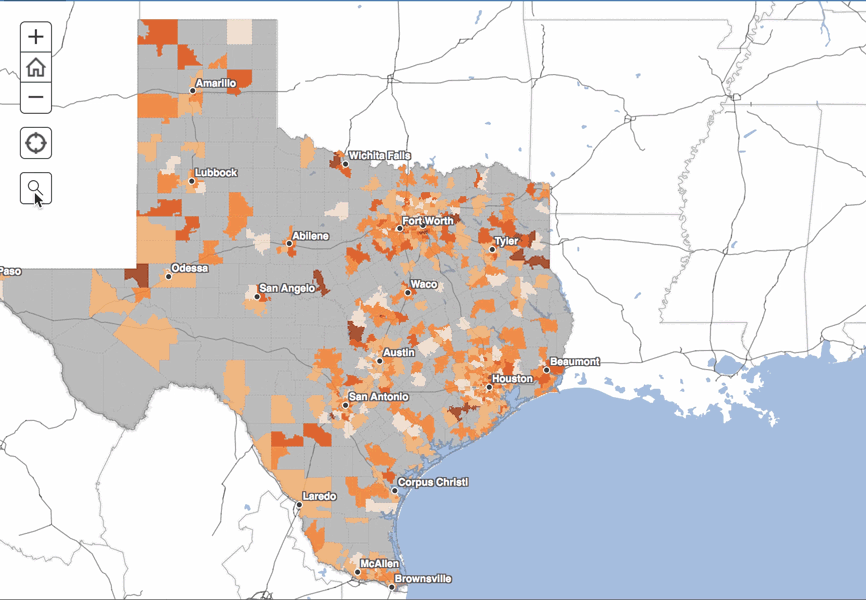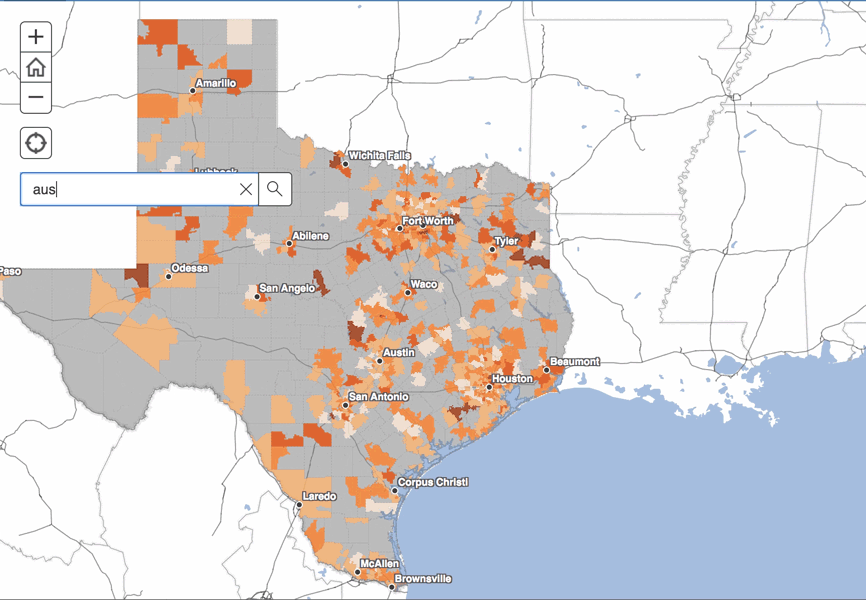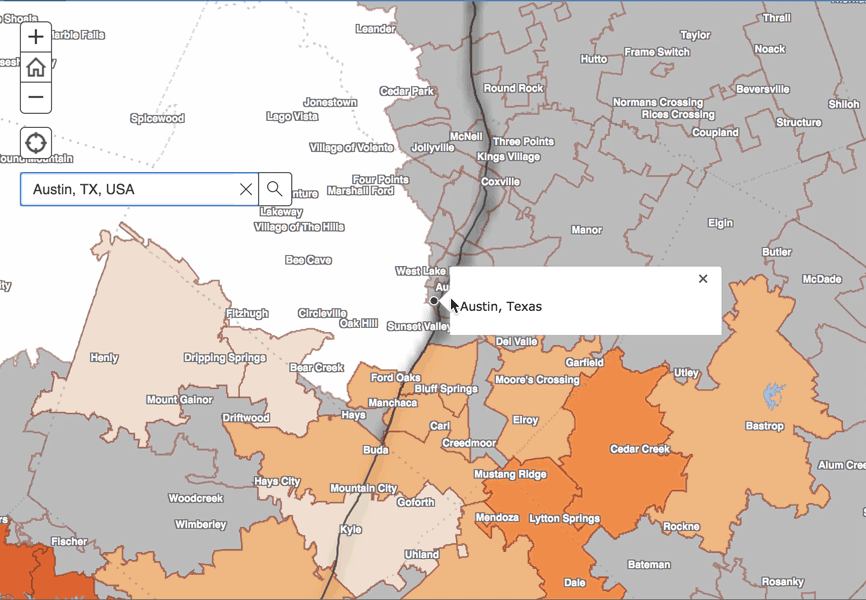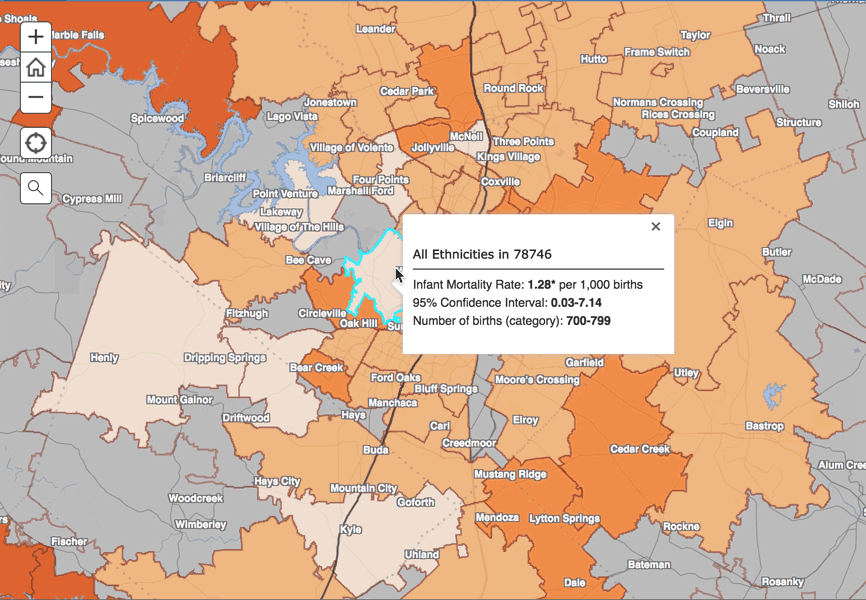
In Fort Worth, for example, the infant mortality rate was over six times higher in the 76164 zip code than in neighboring 76107. Among just black mothers in Houston, there was an eight-fold difference in infant mortality rates across the city. Some zip codes in the state have not experienced an infant death in this four-year time period, whereas others have experienced more than 1 percent of their infants dying before their first birthday.
The zip code level rates were calculated for communities with 400 or more births in this four-year period, and were identified by the mother's zip code of residence at delivery. The data were obtained from the Texas Department of State Health Services (DSHS).
"What this reveals is that the infant mortality picture is dramatically more complex than we knew," said David Lakey, MD, Chief Medical Officer and Vice Chancellor for Health Affairs for UT System. "The state average, which is lower than the national average, obscures zip codes where rates are terribly high. Some of the higher city or county level rates, on the other hand, have obscured the variation within communities, including neighborhoods where rates are very low."
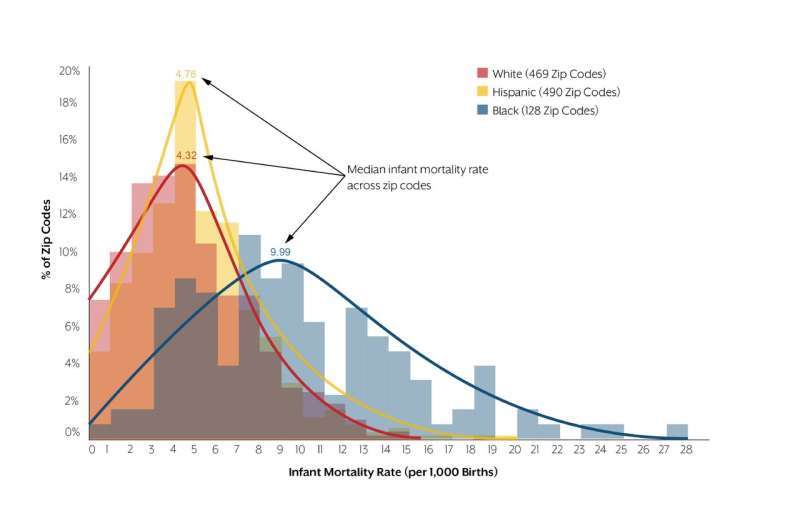
The variations, said Lakey, are both geographic and racial/ethnic. White women in Texas have a relatively low risk of their baby dying within the first year after birth. However, as with the infant mortality rate for all infants, there are significant community-level differences in infant mortality rates among this group. The highest infant mortality rates for white infants were seen outside the major metro areas. For example, Longview and Wichita Falls each had more than one zip code with a white infant mortality rate that was two or more times the overall infant mortality rate in the state.
Of the three major racial/ethnic groups in Texas, Hispanic women have the lowest rate of infant mortality. However, as with white women, infant mortality rates for Hispanic women varied greatly based on where they lived when they were pregnant. In San Antonio, for example, adjacent zip codes 78203 and 78220 both had Hispanic infant mortality rates that were over double the state rate.
Non-Hispanic black families in Texas and the U.S. are disproportionately impacted by infant mortality. However, as for infants of Hispanic and white mothers, mortality rates for infants of black mothers varied across zip codes, even within the same city. Within Houston, for example, mortality rates for infants of black mothers varied eight-fold across zip code, from3.3 to 28.7 deaths per 1,000 births in zip codes 77077 and 77026, respectively.
Although the map shows the wide geographic variation in the state, it does not show why the variation exists. Researchers with UT System will continue to work towards understanding why this variation exists and what can be done to reduce rates overall. UT System is also making public use data files available, as well as other technical information, to facilitate work by other researchers.
"Texas is deeply committed to reducing infant mortality in every community," said Lakey. "Having a lower than average rate, nationally, is not enough, particularly when we know that there are communities where rates are tragically high. What this kind of analysis should enable us to do, moving forward, is to even more precisely identify what best practices to emulate, where to target our interventions, and how best to deploy our resources. We strongly encourage others to make use of this data, and to work on finding solutions. The sooner we can understand why babies are dying, the better off we will all be."
More information:
www.utsystempophealth.org/s/Combined-report-06.pdf
www.utsystempophealth.org/imr-map