Insights into the molecular mechanisms leading to kidney dysfunction in diabetic patients
About one-third of diabetes patients suffer from renal failure. Therefore, understanding the mechanisms linking diabetes to renal damage (diabetic nephropathy) would benefit patients as it would help in developing new therapeutic targets and strategies. Sirtuin 1 (Sirt1) is a protein that is involved in cellular stress responses and has been implicated in diabetic nephropathy. However, the exact role of renal Sirt1 on the pathogenesis of renal damage in diabetes has not been fully elucidated.
Researchers in Japan have previously shown that Sirt1 overexpression can alleviate acute kidney injury in a Sirt1-overexpressing mouse model. The same group has now established the mechanism that links, at least in part, Sirt1 with the pathogenesis of renal damage in diabetes.
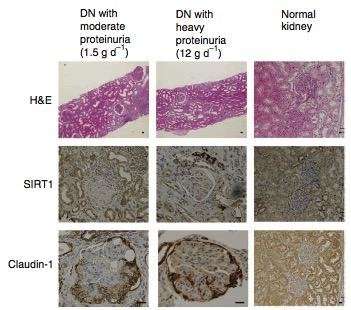
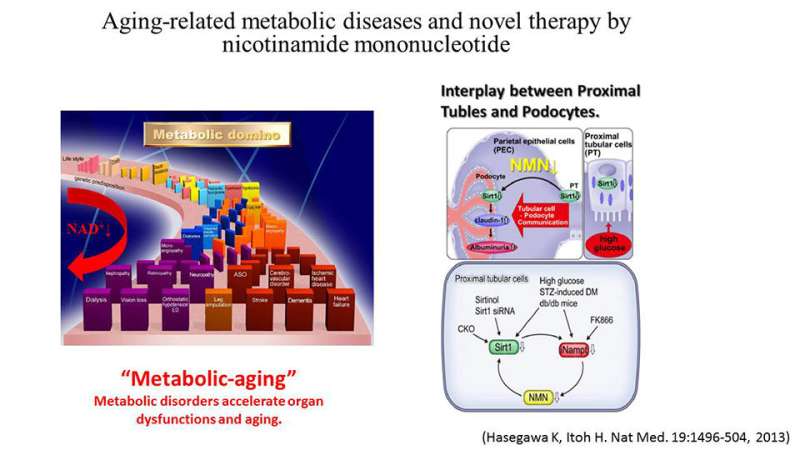
Shu Wakino and colleagues from Keio University, Shizuoka Red Cross Hospital and the Massachusetts Institute of Technology used Sirt1-overexpressing mice, Sirt1 knockout mice and diabetic mouse models to investigate the role of Sirt1 in protecting from diabetes-induced renal damage. Reduction of Sirt1 expression resulted in an increase in Claudin-1 levels and subsequently, albuminuria, which is an early marker of renal damage. The mechanism by which Sirt1 affects the levels of Claudin-1 was found to be through directly epigenetically regulating the expression of the Cldn1 gene. Furthermore, nicotinamide mononucleotide (NMN) was found to mediate the interplay between PTs and podocytes, which are important components of the kidney filtration apparatus, and hence would directly affect albuminuria. Using human renal biopsy samples, the group found that SIRT1 and Claudin-1 levels are also involved in diabetes-related albuminuria in humans.
Taken together the results demonstrate that "Sirt1 in PTs protects against albuminuria in diabetes by maintaining NMN concentrations around glomeruli, thus influencing podocyte function," the authors conclude. Furthermore, since observations in patient samples reflect some of the mouse model results the authors state that "the results of this study could contribute to new therapeutic strategies to prevent diabetes-induced albuminuria."
More information: Kazuhiro Hasegawa et al. Renal tubular Sirt1 attenuates diabetic albuminuria by epigenetically suppressing Claudin-1 overexpression in podocytes, Nature Medicine (2013). DOI: 10.1038/nm.3363