Researchers report inflammation suppression process
Inflammation needs energy An important source for this energy is oxygen, which is indispensable for the cells of the immune system to work properly. Oxygen is an essential element required for cells to survive, but it also adds fuel to the fire of inflammation. Researchers from University of Erlangen-Nuremberg have discovered that the body uses this process to extinguish inflammation. Immune cells are tricked into believing that they lack oxygen, leading them to retreat from the site of the inflammation in order to save energy. These new findings have been published in the journal Nature Communications.
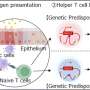
Oxygen sensors in the body measure the concentration of oxygen in the cells. The sensors are activated whenever oxygen levels fall. The most important oxygen sensor in the body is a protein called hypoxia-inducible factor (HIF). Prof. Dr. Aline Bozec demonstrated that increased activation of HIF-1α in immune cells led to a reduction in inflammation. This new research has shed light on a molecular mechanism that keeps serious inflammatory diseases of the human body such as arthritis and multiple sclerosis in check.
"HIF basically acts like a psychotherapist for a certain type of immune cells, the B-lymphocytes," explains Professor Bozec. Under the influence of HIF, B-lymphocytes, which usually have a crucial role to play in the excessive immune response, start to produce the regulating messenger substance Interleukin 10, inhibiting the inflammatory process. By activating HIF, B-lymphocytes seem to switch their allegiance.
The team led by Professor Bozec turned off the oxygen sensor HIF in B cells and observed that this prevented the resolution of inflammation, leading to chronic inflammatory diseases. The results pave the way for new approaches for treating chronic inflammatory diseases such as arthritis or multiple sclerosis using medication to turn off HIF.
More information: Xianyi Meng et al, Hypoxia-inducible factor-1α is a critical transcription factor for IL-10-producing B cells in autoimmune disease, Nature Communications (2018). DOI: 10.1038/s41467-017-02683-x