DOR protein deficiency favors the development of obesity
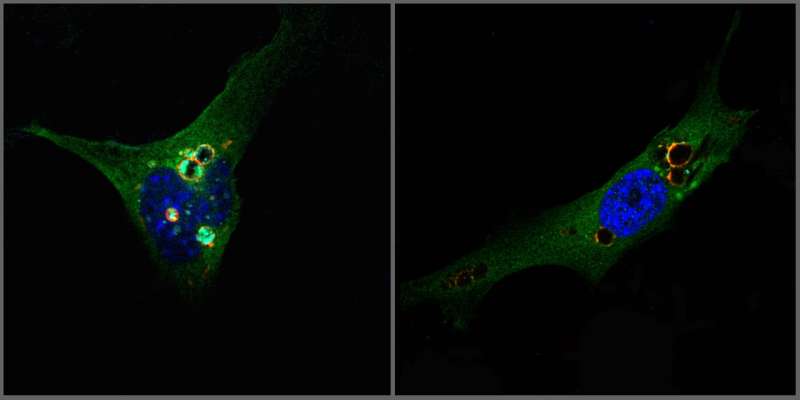
Obesity is a world health problem. Excessive accumulation of fat tissue (adipose tissue) increases the risk of cardiovascular disease, hypertension, diabetes and some types of cancer. However, some obese individuals are less susceptible to these conditions. According to a recent study published by researchers at the Institute for Research in Biomedicine (IRB Barcelona) and CIBERDEM in Nature Cell Biology, deficiency in the protein DOR (also called TP53INP2) stimulates the generation of new adipose cells, which store fat, and leads to a less harmful kind of obesity.
In this study, which was led by Antonio Zorzano, IRB Barcelona researcher, full professor of the University of Barcelona, in collaboration with labs in Gotemburg (Sweden), Tarragona and Girona, the scientists observed that obese patients have low levels of DOR in their adipose tissue.
To further study the link between DOR and obesity, researchers in the Complex Metabolic Diseases and Mitochondria Lab, which headed the study, generated a DOR-deficient mouse model. This animal is characterised by marked obesity in the absence of metabolic complications such as glucose intolerance or inflammation. These features mimic the effect observed in the obese but metabolically healthy patients included in this study. These findings shed light on the mechanism that allows some individuals not to develop the diseases associated with obesity.
Number and volume of fat cells
The number and volume of cells in adipose tissue is particularly relevant with respect to the impact of obesity on health. In this regard, inflammation occurs when a cell increases excessively in size in order to store fat. This inflammation, in turn, leads to insulin resistance. In contrast, if the same amount of fat accumulates in a greater number of cells, the individual will be obese but will be susceptible to fewer associated medical conditions.
Current evidence indicates that, from 20 years of age onward, humans maintain a stable population of adipose cells. So if they lose or gain weight, what changes is the volume of these cells, not their number. However, the new function of DOR revealed in this study shows that a decrease in the levels of this protein in precursor cells programmed to become adipocytes can lead to an increase in the number of fat cells in adult life.
"The solution to obesity does not lie in using treatments to increase the number of adipose cells. Obesity must be prevented," says Zorzano. "But the study helps us to better understand the distinct forms of obesity in humans."
The laboratory is now working on an in-depth analysis of this mechanism to gain a complete understanding of the different types of obesity and to identify potential approaches to prevent and treat this condition.
As described in previous work, DOR is a protein that actively participates in the autophagy processes through which cells recycle damaged or unrequired components in order to ensure optimum function. "Previous studies suggested that the lack of autophagy-related proteins prevented the generation of adipose tissue. However, in the case of the protein DOR, we have observed an increase in the amount of fat accumulated," explains Montserrat Romero, IRB Barcelona researcher and first author of the article, which describes the mechanism through which DOR regulates the transformation of precursor cells into adipose cells.
More information: Montserrat Romero et al, TP53INP2 regulates adiposity by activating β-catenin through autophagy-dependent sequestration of GSK3β, Nature Cell Biology (2018). DOI: 10.1038/s41556-018-0072-9