HIV-1 viruses transmitted at birth are resistant to antibodies in mother's blood
Of the genetically diverse population of HIV-1 viruses present in an infected pregnant woman, the few she might transmit to her child during delivery are resistant to attack by antibodies in her blood, according to new research published in PLOS Pathogens by Amit Kumar of Duke University Medical Centre, North Carolina, and colleagues.
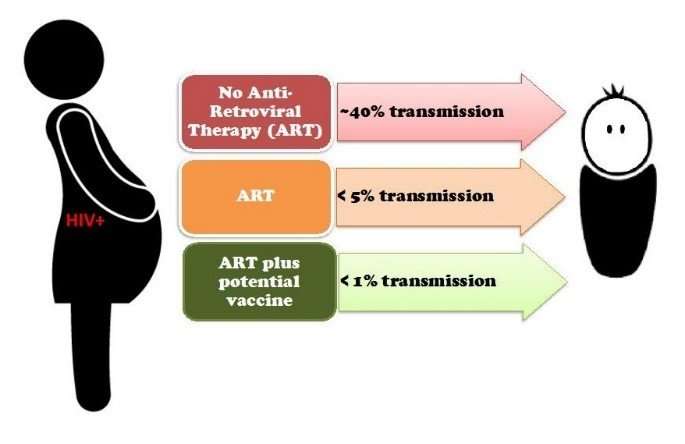
An infected mother can transmit HIV-1 to her child during pregnancy, while breastfeeding, or at the time of delivery. Antiretroviral drugs significantly reduce transmission risk, but these treatments are often not perfectly administered, particularly in resource-poor regions. Better understanding of how HIV-1 viruses are transmitted at delivery could inform new strategies to reduce infant HIV-1 infection.
Previous research has suggested that antibodies—immune system proteins that can attack viruses—in a mother might be less effective against certain genetic variants of HIV-1 in her body, thereby allowing for transmission of resistant viruses to her infant at delivery. However, this research has been inconclusive, so Kumar and colleagues designed a new study to address the question.
The research team analyzed HIV-1 viruses present in blood samples from 16 infants infected at delivery and their mothers; the samples had been collected in the early 1990s in the Women and Infants Transmission Study, before antiretroviral treatments were available. The researchers sequenced the HIV-1 variants, and for each mother-infant pair, they tested the sensitivity of both transmitted and non-transmitted viruses to antibodies concurrently present in the mother's blood.
The analysis revealed that most HIV-1 variants transmitted to the 16 infants at delivery were more resistant to the mothers' antibodies than were non-transmitted variants. However, the transmitted viruses were sensitive to a separate panel of broadly neutralizing HIV-1 antibodies, which can block infection of diverse HIV-1 strains. Genetic analysis uncovered particular sites in the membrane-proximal external region (MPER) and variable loop 3 (V3) of the HIV-1 envelope glycoprotein may be important in mediating maternal antibody resistance.
These findings could help guide development of a new vaccine for pregnant mothers with HIV-1. Such a vaccine would boost maternal antibody attack of HIV-1 variants circulating in the blood, so that transmission risk is reduced when an infant is exposed to maternal blood during delivery.
More information: Kumar A, Smith CEP, Giorgi EE, Eudailey J, Martinez DR, Yusim K, et al. (2018) Infant transmitted/founder HIV-1 viruses from peripartum transmission are neutralization resistant to paired maternal plasma. PLoS Pathog 14(4): e1006944. doi.org/10.1371/journal.ppat.1006944