Medicaid expansion has no negative effect on cardiovascular procedural outcomes: study
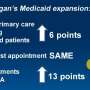
Michigan's Medicaid expansion was associated with more people receiving procedures for coronary artery disease without a negative effect on patient outcomes. That's according to a recent research letter in the Journal of the American College of Cardiology.
"Relative to the 24 months prior to the April 2014 expansion, patients having coronary revascularization procedures within 24 months afterward did equally as well," says lead author Donald Likosky, Ph.D., associate professor of cardiac surgery at the University of Michigan.
"Despite the concern among some that Medicaid patients may be sicker than those with Medicare or private insurance and therefore at higher risk of poor outcomes, quality of care for cardiovascular procedures across Michigan was unchanged following Medicaid expansion."
Few studies have evaluated the impact of Medicaid expansion within the surgical space, researchers behind the letter say.
The team studied two procedure options that improve blood flow to the heart for people with atherosclerosis: an open surgery procedure called coronary artery bypass grafting (CABG) and a minimally invasive treatment called percutaneous coronary intervention (PCI), or angioplasty.
The authors drew from clinically rich information about 7,558 CABG procedures performed at all 33 nonfederal cardiac surgical programs in Michigan, thanks to participation in the Michigan Society of Thoracic and Cardiovascular Surgeons Quality Collaborative, one of Blue Cross Blue Shield of Michigan's Collaborative Quality Initiatives.
The PCI data came from 45,183 procedures at 47 Michigan hospitals participating in another physician collaborative: the Blue Cross Blue Shield of Michigan Cardiovascular Consortium.
Good care and access to ongoing care
Although newly insured patients may not have had the same presenting health conditions or history of primary care utilization as those who previously had insurance, the authors note the increased proportion of patients on Medicaid did not have an impact on patient outcomes.
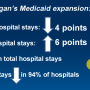
"We found the increase in Medicaid patients in both groups (PCI and CABG) revealed no significant increase in complications, length of stay, or mortality, and these procedures were appropriate procedures," says senior author Richard L. Prager, M.D., a cardiac surgeon and a director of University of Michigan's Frankel Cardiovascular Center. "It is most important to track the effect of these health policy changes."
Co-author Hitinder Gurm, M.D., an interventional cardiologist and associate chief clinical officer at Michigan Medicine, calls the data a "win-win" for Michigan residents and for Michigan hospitals.
"Coronary artery disease that's severe enough to require revascularization can be a huge stress for patients, both personally and financially," says Gurm, who leads BCBSM's cardiovascular consortium, known as BMC2.
"Before Michigan's Medicaid expansion, more people had to manage the challenges of getting care in the uninsured setting. The new process suggests the patients are getting good care and have access to ongoing care."
Need for reporting
According to the Kaiser Family Foundation, 32 states—including Michigan—have expanded Medicaid eligibility. A recent Government Accountability Office report, however, found gaps in individual state reporting after expansion.
"Other states may be limited to counting patients," says Likosky, a member of U-M's Institute for Healthcare Policy & Innovation and director of the PERForm Registry with the Quality Collaborative. "But because of our statewide physician-led effort, we have the ability to evaluate not just volume, but also how the patients did after their procedures."
Meanwhile, other states are expanding or considering expanding their Medicaid programs under the Affordable Care Act using a variety of waivers, such as implementing work requirements.
More information: Donald S. Likosky et al, Association Between Medicaid Expansion and Cardiovascular Interventions in Michigan, Journal of the American College of Cardiology (2018). DOI: 10.1016/j.jacc.2017.12.044