Increased understanding points to new approaches for PTSD prevention and treatment
Recent advances in scientific understanding of how posttraumatic stress disorder (PTSD) develops and persists may lead to more effective treatment and even prevention of this debilitating disorder, according to the May/June special issue of Harvard Review of Psychiatry.
A growing body of evidence helps psychiatrists to understand the aspects of brain structure and function involved in PTSD, informing efforts to interrupt the processes leading to the development of PTSD symptoms in traumatized individuals, according to an introductory article by Guest Editor Kerry J. Ressler, MD, PhD, of McLean Hospital/Harvard Medical School, Belmont, Mass. Dr. Ressler writes: "PTSD, while one of the most recently defined syndromes in psychiatry, may also be one of the earliest to benefit from progress in neurobiology and advances in translational approaches to brain function and behavior."
Understanding Dysfunctional Fear and Emotional Processes May Improve Treatment for PTSD
Dr. Ressler notes that patients with PTSD have "characteristic reexperiencing, avoidance, and hyperarousal symptoms," which can persist for months or years after exposure to traumatic events. Posttraumatic stress disorder affects about 6 percent of the population, but the rate is much higher in groups exposed to severe trauma, such as combat veterans, refugees, and assault victims.
Although PTSD is at least partly genetic, it also depends on personal history of trauma in childhood and adulthood, as well as psychological factors linked to mediation of fear and regulation of emotions. "Therefore, PTSD is among the most likely of psychiatric disorders to be understood from the perspective of environmental influences interacting with biological vulnerability," according to Dr. Ressler. The special issue provides expert updates in four key areas related to the development, diagnosis, and management of PTSD:
- Neurophysiology. Scientific understanding of human fear responses provides important insights into how PTSD develop and persists. The mechanism of "fear extinction" - in which learned fear is suppressed by new learning - is highly relevant to PTSD and its treatment. Dr. Ressler notes that effective treatments for PTSD, particularly exposure therapy, are based on the mechanisms of fear extinction.
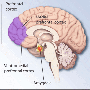
- Neuroimaging. Research has also made strides in identifying the brain structures and functions involved in emotion dysregulation of PTSD. Studies have identified biomarkers of these dysregulated processes, including abnormal functioning of the body's stress responses and dysfunction of a brain areas called the hippocampus and amygdala, which are involved in memory and emotional responses. These discoveries may point toward treatments targeting stress hormones and functioning of these brain regions.
- Resilience. The concept of resilience - the ability to adapt successfully to trauma or threat - is being studied to explain why some traumatized individuals develop PTSD symptoms while others do not. Interventions to promote resilience have potential not only as a treatment for people with PTSD, but for also preventing it in populations at risk of trauma.
- Evidence-based treatments. The special issue concludes with a review and update of evidence behind the range of "reasonably effective" treatments for PTSD. Psychotherapy approaches address the underlying dysfunctions of fear extinction and emotion regulation. A class of antidepressants (selective serotonin reuptake inhibitors) are the only FDA-approved medications for PTSD, but many other drugs may be used off-label to treat specific symptoms.
While current treatments do address the underlying mechanisms of PTSD, many patients do not improve or continue having symptoms, while others might have a better response to individualized treatment approaches. "Advances in neurobiology and behavioral science are needed for truly targeted, innovative, robust treatments and preventions," Dr. Ressler concludes.
More information: Meredith E. Charney et al. Evidenced-Based Treatment of Posttraumatic Stress Disorder, Harvard Review of Psychiatry (2018). DOI: 10.1097/HRP.0000000000000186