How lessons from childhood cancer care could improve adult cancer care
A cancer diagnosis is a firestorm that turns lives upside down. It may not be life-ending, but it almost always is life-changing.
Few life experiences are crueler than childhood cancer, but this blatant unfairness motivates some of the best, kindest and most heartfelt medical care. Clinicians in adult oncology can learn a lot from pediatric cancer practices.
Based on our service quality research in more than a dozen cancer centers and hospitals in three countries, here are three ways we found pediatric cancer care can improve service delivery in adult oncology. With more than 1.6 million people diagnosed with cancer in 2017 in the U.S. alone, the stakes are high.
Empathetic creativity
Empathy in medical care involves nonjudgmental recognition of anxiety, fear and other emotions and providing genuinely caring responses to them. To respond effectively to a child who one day is playing with friends and the next day is undergoing an MRI exam requires empathy-driven creativity.
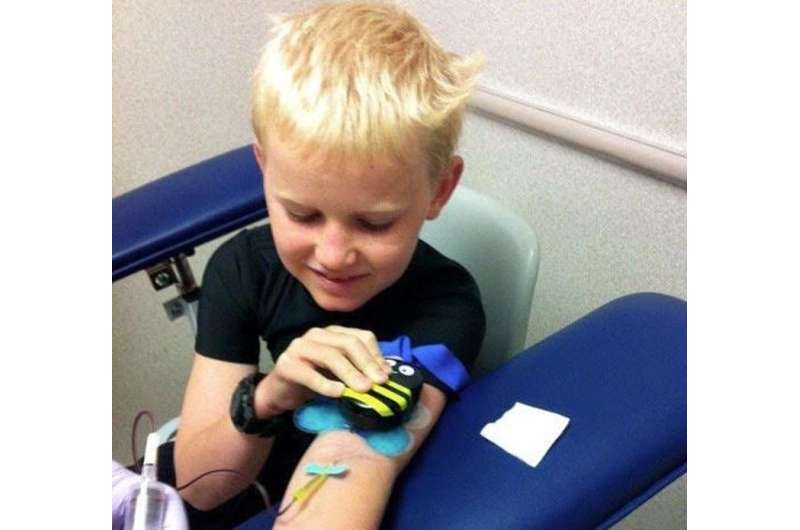
Being unprepared for the unfamiliar is a huge stressor, and pediatric cancer care providers have adopted clever ways to reduce the fear of a procedure or treatment. If a child fears needles, a child life specialist may teach the patient to paint with a syringe. Patients may role play chemotherapy by infusing a stuffed animal outfitted with a central line or port, such as the Chemo Duck. Similarly, Buzzy Bee, a bee-shaped device that vibrates, relieves pain by sending sensations down the same neural pathways taken by pain from a shot or IV placement.
At Monash Children's Hospital, in Melbourne, Australia, a patient who needs an MRI exam first meets with a child life specialist who explains the machine and shows an interactive cartoon about the exam. The child then plays with a teddy bear "patient" on a small mock MRI machine. Then the child gets on a real MRI machine, which has been disabled for "practice runs," and goes through the getting ready sequence. The child selects a movie to watch, can change the ceiling color, and chooses images to project on the walls.
If the child copes well with the practice run, he or she may be able to undergo the actual exam without general anesthesia, which reduces risk and cost.
Pediatric cancer centers commonly use various forms of play to distract patients from their fears. Boston Children's Hospital has activity rooms with child life specialists, patient entertainment centers, a Clown Care Unit, and the PawPrints Dog Visitation Program. At Australia's Peter MacCallum Radiation Center pediatric patients and their siblings choose superhero costumes for appointments and a movie. A film crew creates a superhero movie about each child's treatment journey, which the child receives after treatment.
Family-centered care
In pediatric cancer care, the child's family is a primary source of support and, for younger patients especially, decision-making. Family-centered care, inclusive of the patient's family in the care process, is guided by these principles: information sharing, respect and honoring differences, partnerships and collaboration, negotiation, and care in the context of family and community. The care team becomes "part of the family," and they take an interest in the families' lives beyond treatment.
Parents have to be advocates, protectors, encouragers, confidence-builders and caregivers for their child, while they are dealing with their own fears. Parents may have to make difficult decisions, such as whether or not to continue "curative" treatments for what in some instances is almost surely an incurable cancer. In pediatric cancer, families are more likely to be involved in treatment planning as care team members than in adult cancer care.
An 11-year-old girl we'll call Susan had a brain tumor. The clinical team watched the tumor for three years. It didn't grow, until it did slightly. The doctors wanted to remove it immediately, although Susan had no symptoms and the tumor was not life-threatening. Susan's mom asked to postpone surgery until school ended. The doctors moved the surgery date. Susan's mom was an active member of the care team, which is the norm in pediatric oncology.
Ben, a 4-year-old cancer patient, spent long periods in the hospital. Certain avoidable stressors became evident, so Ben's parents and clinical staff drafted a list of his likes and dislikes. Ben's "treatment rules" were placed on the door to his room, including silence during procedures, no crowds of people in his room, being as quick as possible, and giving Ben as much control as possible during procedures.
Compassionate volunteerism
Embedded in every service role is discretionary effort, or the difference between the amount of effort one brings to the work and the minimum amount necessary to avoid adverse consequences. Discretionary effort is, in effect, voluntary; it is "extra effort." The emotional nature of pediatric oncology fosters compassion and staff volunteerism, a potent combination of attitude and behavior.
Let's return to Susan in the hospital a few hours before brain surgery when she was 14:
"When Ava, my nurse, came by before surgery she looked me in the eye and said, 'Susan, I am going to braid your hair back so that we only shave what we need.' What Ava did shaped how I viewed myself every time I glanced in the mirror during recovery and when I walked into school surrounded by normal girls. Ava probably doesn't remember braiding my hair, but that moment has stuck with me for the last six years."
Susan, now a healthy 20-year-old, wrote these words for a college paper. Ava didn't have to braid Susan's hair. Braiding hair wasn't in her job description. But she did it, and it meant everything to Susan. Compassionate volunteerism can go a long way.
Empathetic creativity, family-centered care and compassionate volunteerism offer a life vest in a sea of suffering when cancer strikes. Common in pediatric cancer care, these guideposts are practical for all cancer patients.