Carrying stand-by antibiotics fosters careless antibiotic use among travelers
Travellers carrying standby antibiotics take them more often than those traveling without such drugs. Antibiotics packed in the bags encourages misuse for mild and moderate diarrhoea, i.e., cases not requiring medication.
Increasing antimicrobial resistance, primarily caused by excessive and uncontrolled use of antibiotics, is a globally recognized severe threat to human health. Returning home, approximately every third traveller to the tropics carries intestinal multiresistant bacteria. The risk of having contracted such bacteria is doubled by taking antibiotics during the journey.
Seeking a means to avoid unnecessary antibiotic use, a study was carried out jointly by the University of Helsinki, the Helsinki University Hospital, and the Aava Travel Clinic, aiming to identify factors increasing antibiotic use among travellers.
"To cut down unnecessary antibiotic use, the underlying factors need to be explored," says Anu Kantele, professor at the University of Helsinki and the project lead.
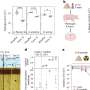
The study comprised 316 prospectively recruited subjects who had contracted travelers' diarrhoea during their visit to the tropics. Of the 316 participants, 53 had brought stand-by antibiotics from Finland. The most common reason for antibiotic use was diarrhoea, the most prevalent disease among travellers to the tropics, followed by respiratory infections.
As risk factors associated with use of antibiotics, the study identified carrying stand-by antibiotics, vomiting, diarrhoea disrupting or preventing daily activities and contacts with local health care at the destination.
Of those carrying vs not carrying stand-by antibiotics, 34 percent vs. 11 percent resorted to antibiotic therapy. Severe diarrhoea was treated with antibiotics similarly in the two groups, yet carriers of stand-by antibiotics also used them for mild and moderate diarrhoea. "According to the Finnish guidelines, antibiotics should be used for diarrhoea patients with a high fever or an exceptionally severe disease or deteriorating condition, or if they have an underlying disease which may become aggravated," says Kantele.
"In other words, antibiotics should only be used to treat severe diarrhoea, whereas for mild and moderate disease, fluid therapy and non-antibiotic drugs suffice." Rather than the severity of diarrhoea, the factor determining recourse to antibiotics was travelers' subjective experience of disturbance of daily activities.
"Physicians in Finland and elsewhere should give up routinely prescribing antibiotics against travelers' diarrhoea," Kantele concludes.
More information: Katri Vilkman et al, Stand-by antibiotics encourage unwarranted use of antibiotics for travelers' diarrhea: A prospective study, Travel Medicine and Infectious Disease (2018). DOI: 10.1016/j.tmaid.2018.06.007