Pediatric NEXUS head CT DI reliably guides blunt trauma imaging decisions
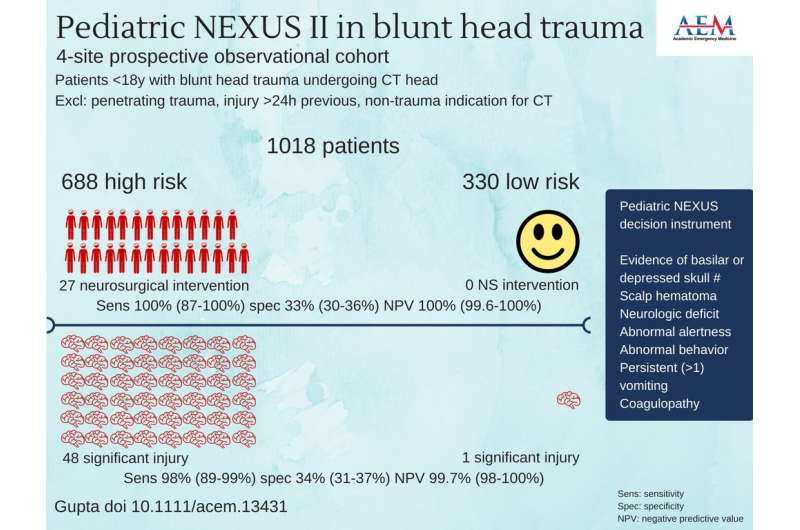
The Pediatric NEXUS Head Computed Tomography (CT) Decision Instrument (DI) reliably identifies blunt trauma patients who require head CT imaging and could significantly reduce the use of CT imaging. Those are the findings of a to be published in the July issue of Academic Emergency Medicine, a journal of the Society for Academic Emergency Medicine (SAEM).
The lead author is Malkeet Gupta MD, MS, assistant clinical professor in the Department of Emergency Medicine at UCLA.
The study by Gupta et al, validates the NEXUS Head Computed Tomography Decision Instrument in pediatric patients and provides clinicians with a highly sensitive tool to guide selective imaging decisions in blunt head injury patients. Unlike other decision instruments, the decision instrument asks providers to use clinical judgment to identify low-risk patients who need no imaging and then to apply the decision instrument to further reduce the planned imaging. This "judgment first, decision instrument second" approach may decrease head CT utilization in low-risk pediatric populations by up to 34%.
The findings of the study are discussed with Dr. Gupta in the featured episode of SGEM Hop (Skeptics Guide to EM Hot Off the Press).
Joshua S. Broder, MD, director of the Emergency Medicine Residency Program and vice-chief for education in the Division of Emergency Medicine at Duke University School of Medicine, commented on the study:
"This study provides another tool in our armamentarium for assessing pediatric patients with traumatic head injury and has the potential to reduce CT utilization. Some elements of the decision instrument are poorly predictive; scalp hematoma alone, for example, does not indicate substantial risk of injury. Changes in nomenclature could help. For example, the term 'high-risk' may not accurately describe patients who fail one or more measures on the instrument, as the rate of significant head injury in this group was approximately 7%. 'Non-low risk' or 'intermediate risk' may more accurately describe some patients who might be safely observed without imaging."
More information: Malkeet Gupta et al, Validation of the Pediatric NEXUS II Head Computed Tomography Decision Instrument for Selective Imaging of Pediatric Patients with Blunt Head Trauma, Academic Emergency Medicine (2018). DOI: 10.1111/acem.13431