Social Impact Bonds have a role but are no panacea for public service reform
Led by the Policy Innovation Research Unit at the London School of Hygiene & Tropical Medicine with RAND Europe, and funded by the NIHR Policy Research Programme of the Department of Health and Social Care, the findings show that policymakers should focus on the components within SIBs that show promise in developing outcome-based contracting, such as personalised support to clients, and greater flexibility and innovation in service delivery, while avoiding the notion that SIB offer the only way forward for such contracting.
Despite claims that SIBs should generate rich quantitative information on the costs and outcomes of SIB-funded and non-SIB services, in practice the researchers were unable to access suitable quantitative data to make this comparison.
SIBs are a relatively new type of payment for performance contract where public sector commissioners partner with private or third sector social investors to fund interventions that seek to tackle complex social issues.
This report is the first to examine the impact of the SIB financing mechanism on each of the main groups of participants, including service providers.
Professor Nicholas Mays, Professor of Health Policy at the London School of Hygiene & Tropical Medicine, said: "The main demonstrable success of SIB projects in health and social care has been in helping marginalised groups who had, previously, been neglected by public services. It is much less clear that SIB-related services for other groups, such as people with chronic health conditions, have led to marked improvements in health."
The study evaluated nine projects across England, collectively known as the SIB 'Trailblazers', that received seed funding from the Government's Social Enterprise Investment Fund to develop and potentially implement a SIB. The team analysed Trailblazer plans and contracts, conducted interviews with national policy makers and local participants in Trailblazer SIBs (commissioners, investors, SIB specialist organisations and providers), as well as local participants in comparable non-SIB services.
The SIBs funded a wide range of different interventions for different clients: older people who are socially isolated; people with multiple chronic health conditions; entrenched rough sleepers; adolescents in care; and people with disabilities requiring long-term supported living.
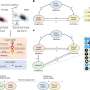
Three models of SIB were identified: the Direct Provider SIB; SIB with Special Purpose Vehicle; and the Social Investment Partnership. Each allocated financial risks differently, with providers bearing more of the financial risk in the Direct Provider model than in the others.
Frontline staff were more aware of the financial incentives associated with meeting client outcomes in the Direct Provider model than in the Special Purpose Vehicle model. Providers in the Trailblazers were more outcome-focused than providers of comparable non-SIB services.
Despite this, the up-front financing of providers by investors tended to be provided in instalments related to hitting volume and/or throughput targets rather than improvements in client outcomes. The bulk of the subsequent payments to investors for achieving targets came from central government and sources such as the Big Lottery rather than from local commissioners.
Only one Trailblazer reported having made any cashable savings during the evaluation period as a result of its SIB-financed interventions. Typically, the planning of the SIB services and subsequent oversight were better resourced, and the services more flexibly provided than in similar non-SIB services.
Professor Mays said: "Our research provides important information for governments looking for new financing mechanisms for health and care. So far at least, cashable savings from SIBs, despite early hopes and rhetoric, remain unproven. Policymakers should learn from different models but SIBs are no panacea for better commissioning of health and care services."
The researchers conclude that SIBs, as currently conceived, may have a role in specific circumstances, especially where outcomes are uncontroversial, easily attributable to the actions of the provider and easily measured but are unlikely to be widely applicable in public services.
The authors acknowledge limitations of the study including that, with the exception of one Trailblazer which ended during the evaluation, the other four operational SIBs were evaluated during their early to mid-period of implementation, making it possible that the performance of these projects will change before they conclude in two to five years' time.
More information: Publication: Alec Fraser, Stefanie Tan, Kristy Kruithof, Megan Sim, Emma Disley, Chris Giacomantonio, Mylene Lagarde and Nicholas Mays. Evaluation of the Social Impact Bond Trailblazers in Health and Social Care