Risk adjusting for race and poverty bolsters rankings of some hospitals
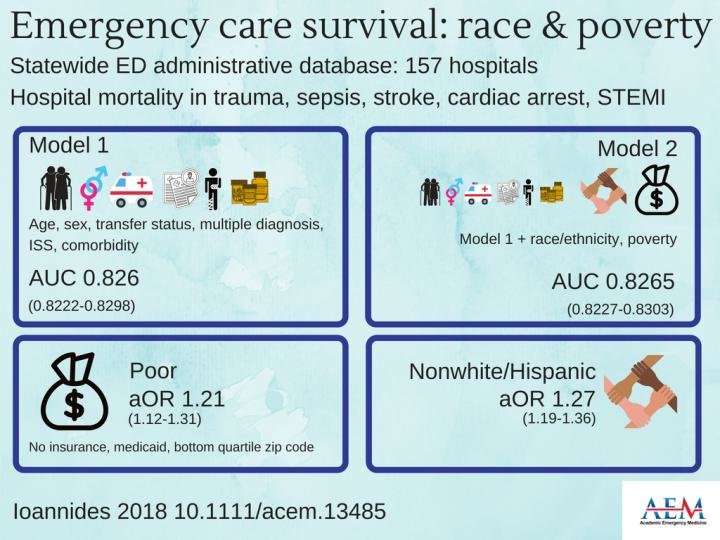
Sociodemographic risk adjustment of emergency care-sensitive mortality improves apparent performance of some hospitals treating a large number of nonwhite, Hispanic, or poor patients. That is the finding of a study published in the August 2018 issue of Academic Emergency Medicine (AEM), a journal of the Society for Academic Emergency Medicine (SAEM).
The lead author of the study is Kimon L. H. Ioannides MD, Assistant Professor, Clinical Pathology and Laboratory Medicine, Lewis Katz School of Medicine Temple University, Philadelphia.
The study, by Ioannides et al, demonstrate substantial potential financial benefits from sociodemographic adjustment for safety net hospitals taking care of vulnerable patients. Within the broader debate about the role of safety net hospitals, the findings also provide key evidence on potential effects of payment reform on nonemergency care and on hospital markets more generally.
Ioannides et al recommend including sociodemographic adjustment in payment models to avert harm to safety net hospitals and vulnerable patients, but caution that close monitoring, reporting of adjustment trends (including other comorbidities), and robust data transparency (including rankings stratified by sociodemographics) are required to avoid exploitation of these adjustments.
Lynne D. Richardson, MD, Professor of Emergency Medicine, Professor of Population Health Science and Policy, and System Vice Chair of Emergency Medicine at The Icahn School of Medicine at Mount Sinai in New York City, commented:
"This analysis by Ioannides et al adds to the growing evidence that traditional approaches to risk adjustment do not adequately account for the impact of persistent and pervasive societal inequities on observed health outcomes. We must continue to refine and improve the quality metrics used to evaluate hospital and physician performance by integrating important social determinants of health into our risk adjustment models."
More information: Kimon L. H. Ioannides et al, Measuring Emergency Care Survival: The Implications of Risk Adjusting for Race and Poverty, Academic Emergency Medicine (2018). DOI: 10.1111/acem.13485















